Abstract
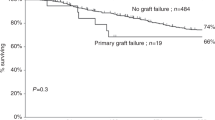
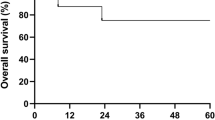
We retrospectively compared the incidence and clinical characteristics of cGVHD in 37 allo-PBT recipients transplanted between July 1994 and October 1996 and 37 historical control allo-BMT recipients in a case- control study. All patients received a first unmanipulated transplant, graft from an HLA-identical sibling donor, with CsA-MTX GVHD prophylaxis and survived more than 100 days after transplant. PBT and BMT groups were well matched for age, grade of acute GVHD, male patients grafted from female donors, and phase of disease. The median CD34+ and CD3+ cell numbers infused in the PBT group were 5.2 × 106/kg and 307 × 106/kg, respectively. The median time to an ANC greater than 0.5 × 109/l was 16 days (range 11–22) after PBT and 22 days (range 14–36) after BMT (P < 0.001). the median time to a platelet count greater than 20 × 109/l was 15 days (range 6–43) after PBT and 28 days (range 12–68) after BMT (P < 0.001). median follow-up was 12.3 months (range 5.4–30.3) and 58.7 months (range 4–122.3), for patients receiving pbt and bmt, respectively. seventeen out of 37 (46%) pbt recipients, vs nine out of 37 (24%) BM recipients developed cGVHD. Actuarial probability of cGVHD at 1 year was 59% (95% CI, 39–79) in the PBT group vs 27% (95% CI, 12–42) in the BM group (P = 0.01). Cumulative incidence estimate of cGVHD was 51% and 25%, for patients receiving PBT and BMT respectively (P = 0.03). Clinical characteristics of cGVHD and response to therapy were similar in both groups, except for a higher incidence of de novo cGVHD in the PBT group. Our results suggest that as compared with BMT, PBT may result in an increased incidence of cGVHD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Consortia
Rights and permissions
About this article
Cite this article
Solano, C., Martinez, C., Brunet, S. et al. Chronic graft-versus-host disease after allogeneic peripheral blood progenitor cell or bone marrow transplantation from matched related donors. A case-control study. Bone Marrow Transplant 22, 1129–1135 (1998). https://doi.org/10.1038/sj.bmt.1701500
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1701500
Keywords
This article is cited by
-
Superior GVHD-free, relapse-free survival for G-BM to G-PBSC grafts is associated with higher MDSCs content in allografting for patients with acute leukemia
Journal of Hematology & Oncology (2017)
-
Chronic Graft Versus Host Disease in Acute Leukemia Patients Undergoing Allogeneic Hematopoietic Stem Cell Transplant: Analysis of Risk Factors, Pattern and Long Term Outcome
Indian Journal of Hematology and Blood Transfusion (2016)
-
Repeated course of rituximab for treatment of nephrotic syndrome in patients with chronic GVHD
Bone Marrow Transplantation (2010)
-
G-CSF increases the number of peripheral blood dendritic cells CD16+ and modifies the expression of the costimulatory molecule CD86+
Bone Marrow Transplantation (2006)
-
Increased acute GvHD and higher transplant-related mortality in non-caucasians undergoing standard sibling allogeneic stem cell transplantation
Bone Marrow Transplantation (2006)