Abstract
This study aimed to evaluate the validation of the leptin receptor-deficient mice model for secondary osteoporosis associated with type 2 diabetes mellitus (T2DM) at bone micro-architectural level. Thirty three 36-week old male mice were divided into four groups: normal control (db/m) (n = 7), leptin receptor-deficient T2DM (db/db) (n = 8), human C-reactive protein (CRP) transgenic normal control (crp/db/m) (n = 7) and human CRP transgenic T2DM (crp/db/db) (n = 11). Lumber vertebrae (L5) and bilateral lower limbs were scanned by micro-CT to analyze trabecular and cortical bone quality. Right femora were used for three-point bending to analyze the mechanical properties. Trabecular bone quality at L5 was better in db/db or crp/db/db group in terms of bone mineral density (BMD), bone volume fraction, connectivity density, trabecular number and separation (all p < 0.05). However the indices measured at proximal tibia showed comparable trabecular BMD and microarchitecture among the four groups. Femur length in crp/db/db group was significantly shorter than db/m group (p < 0.05) and cortices were thinner in db/db and crp/db/db groups (p > 0.05). Maximum loading and energy yield in mechanical test were similar among groups while the elastic modulus in db/db and crp/db/db significantly lower than db/m. The leptin-receptor mice is not a proper model for secondary osteoporosis associated with T2DM.
Similar content being viewed by others
Introduction
Type 2 diabetes mellitus (DM) is a major metabolic disorder that causes profound medical and socioeconomic burden. It currently affects about 382 million adults worldwide and it is projected to reach 592 million by 20301. Type 2 DM is associated with a series of complications that can affect multiple organ systems, including the bone. A recent meta-analysis of 12 studies shows that adults with type 2 DM are at a heightened risk of hip fracture with a relative risk of 1.72. Paradoxically, areal bone mineral density (BMD) measured by dual-energy X-ray absorptiometry (DXA) is found to be normal or higher in these patients3,4,5, leading to the hypothesis that type 2 DM is associated with material and microstructural deficits of the bones which contribute to the increased fracture risk6,7.
The underlying mechanism for type 2 DM-induced osteoporosis is still elusive. It may involve excessive accumulation of advance glycosylation end-products as a result of hyperglycemia, increased fat deposition at the bone marrow and impaired osteoblast function8,9,10,11,12,13. C-reactive protein (CRP) is an acute-phase reactant produced primarily in the liver under the stimulation of pro-inflammatory cytokines such as interleukin-6 and tumor necrosis factor-α. Elevated CRP levels represent a state of low grade inflammation which has been shown to disturb bone metabolism and has been shown to be associated with enhanced risk of fragility fracture in the general population14,15,16,17. A number of studies have described elevated CRP levels in patients with type 2 DM18,19,20. Whether bone fragility in type 2 DM is a result of elevated CRP levels is yet to be determined.
Leptin receptor-deficient (db/db) mouse was reported as an animal model of type 2 DM21. These animals had autosomal recessive mutation in the leptin receptor and had features typical of type 2 DM, including hyperphagic, obese and hyperglycemia. The aim of this study was to evaluate bony statues at microarchitectural level to determine whether leptin receptor-deficient mice model was a potentially valid animal model for type 2 DM-associated secondary osteoporosis.
Materials and Methods
Groups
Thirty three 36-week old male mice purchased from Laboratory Animal Services Centre of the Chinese University of Hong Kong were used and grouped into 4 groups: normal control mice (db/m) (n = 7), leptin receptor knock-out type 2 DM mice (db/db) (n = 8), human CRP transgenic normal control mice (crp/db/m) (n = 7) and human CRP transgenic db/db type 2 DM mice (crp/db/db) (n = 11). All animals were sacrificed by injecting excessive pentobarbital after being anesthesia by ketamine solution at 36 weeks. Body weight of all the mice was recorded. Lumbar vertebrae 4 to 6 (L4–6) and bilateral lower limbs were harvested. Right femora were preserved in saline before three-point bending test while the rest of the samples were fixed with formalin and kept in 70% ethanol before use. The study was conducted with the approval from the Animal Experimentation Ethics Committee of the Chinese University of Hong Kong (AEEC No. 09/027/MIS) and was conducted according to the approved guideline.
Evaluation of bone architecture by micro-CT
For evaluation of trabecular bone density and microarchitecture, vertebral body L5 and a section of 850 μm in length of proximal tibia below the growth plate were scanned with a micro-CT system (Micro CT 40, SCANCO Medical, Switzerland) at a voltage of 70 keV in a spatial resolution of 10 μm for animal experimental studies. Measurements were repeated for each sample and the mean values were used for analysis. Volumetric BMD, ratio of bone volume and total volume (BV/TV), trabecular bone number (Tb.N), trabecular bone thickness (Tb.Th), trabecular bone separation (Tb.Sp) and structural model index (SMI) were collected and analyzed. SMI is an index for determining the plate- or rod-like geometry of trabecular structures. For an ideal plate and rod structure, the SMI value is 0 and 3, respectively. For a structure with both plates and rods of equal thickness the value lies between 0 and 3, depending on the volume ratio of rods and plates22. For evaluation of cortical bone architecture, a section of 900 μm of the middle shaft of the right femur which comprised pure cortical bone was scanned with the same micro-CT system with settings as above. The following parameters were collected: the diameter of the cross-section area, thickness of the cortical bone.
Mechanical test
A material test machine (H25KS, Hounsfield Test Equipment Ltd.UK) with a 25N load cell was used for testing mechanical properties of the femur. The left femur was positioned horizontally with the anterior surface upwards and centered on the supports with 10 mm apart. Load was applied at the mid-shaft constantly with displacement rate of 5 mm/min and directed vertically to mid-shaft with anterior surface upward. After testing to failure, the force-displacement curves were recorded. Also the stress-strain curve was obtained by being normalized by stressed area. This conversion would be calculated automatically by the built-in software QMAT (QMAT Professional; Tinius Olsen, Inc. Horsham, PA, USA). Failure force (N), elastic modulus (E-modulus = stress/strain), energy at yield (integration of the total area under the stress-strain curve) were obtained and analyzed by a built-in software QMAT based on our previous established protocols23.
Statistical analyses
All data were expressed as mean and standard deviation. Between-group differences were analyzed by one-way analysis of variance (ANOVA). All statistical analyses were performed by Statistical Package for the Social Sciences (SPSS, version 17.0, Chicago, IL, US). A p-value less than 0.05 was considered statistically significant.
Results
Leptin receptor knock-out type 2 DM leads to higher body weight
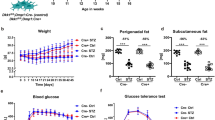
Human CRP transgene did not affect the body weight. Body weight was comparable between db/m and crp/db/m mice and between db/db and crp/db/db mice. Compared with db/m mice, db/db and crp/db/db mice had 58.5% and 70.7%, respectively, significantly higher body weight (both p < 0.05). Compared with crp/db/m mice, body weight was also significantly higher in db/db and crp/db/db mice (both p < 0.05) (Fig. 1).
Leptin receptor knock-out type 2 DM mice have higher trabecular bone density and better microarchitecture at L5
In general, indices of trabecular bone microarchitecture at L5 were comparable between db/m and crp/db/m mice, except that connectivity density was significantly higher in crp/db/m (Fig. 2). Compared to db/m mice, BMD, BV/TV, connectivity density, Tb.N and were all significantly higher and Tb.Sp significantly lower in db/db or crp/db/db mice (all p < 0.05) (Fig. 2). The largest difference was seen in connectivity density, which was 5.6 times and 6.2 times higher for db/db and crp/db/db mice, respectively. Tb.Th did not differ among the four groups. The average SMI of db/db and crp/db/db mice was 1.202 and 0.889, respectively, which was lower than those of db/m (1.995) or crp/db/m (1.671) mice. This indicated that the trabeculae at L5 contained more plate-like structure for db/db and crp/db/db mice while more rod-like structure for db/m and crp/db/m mice (Table 1). Indices of trabecular bone were comparable between db/db and crp/db/db mice. The 3D images of trabecular bone in L5 are shown in Fig. 3 where the images show particularly denser and better connected trabeculae in db/db and crp/db/db mice compared with db/m and crp/db/m mice.
Comparable trabecular bone density and microarchitecture at the proximal tibia among groups
In contrast to the findings at L5, in general, indices of trabecular bone microarchitecture at the proximal tibia did not differ significantly among the four groups of mice (Fig. 4). BMD was also found comparable among groups. There was a trend towards a lower BV/TV in db/db (mean: 0.086) and crp/db/db (0.077) mice compared with db/m (0.112) and crp/db/m (0.095) mice. Connectivity density tended to be lower in crp/db/m and crp/db/db. However, these differences did not reach statistical significance. Tb.N and Tb.Sp did not differ significantly among groups. Tb.Th was similar between db/db and crp/db/db mice with average Tb.Th being 0.048 mm for both groups, respectively. Significant difference in Tb.Th was only found between db/m and crp/db/db mice. SMI at proximal tibia ranged from 2.08 to 2.48, with comparable SMI among groups, representing the trabecular bone at this region tended to contain more rod-like structure (Table 1). Figure 3 shows the 3D image of trabecular bone at the proximal tibia. The images show trabecular bone with similar density and connectivity among the four groups.
Comparable cortical bone architecture at mid femoral shaft and mechanical properties among groups
The length of the femur was 8.55% (p < 0.05) significantly shorter in crp/db/db mice than in db/m mice (Fig. 5). Cross-sectional area and cortical thickness of the femur tended to be lower in db/db and crp/db/db group compared with db/m and crp/db/m mice but the differences were not statistically significant (p > 0.05). Group-wise differences in the maximum loading and energy yield were not significantly different (all p > 0.05) (Fig. 5). Compared with db/m mice, elastic modulus was 9.75% and 8.67% significantly lower (both p < 0.05) in db/db and crp/db/db mice, respectively.
Discussion
In this study, we investigated the bone density and microarchitecture at the spine and limb in a type 2 DM mice model. Leptin receptor knock-out type 2 DM led to significantly higher body weight and human CRP gene did not affect body weight as body weight was comparable between db/m and crp/db/m mice and between db/db and crp/db/db mice. Assessment by micro-CT revealed high bone mass phenotype at L5 in type 2 DM mice (db/db) and type 2 DM mice with human CRP transgenic gene (crp/db/db), evidenced by significantly higher trabecular BMD, BV/TV, connectivity density, Tb.N and lower Tb.Sp. At the proximal tibia, Tb.Th was significantly lower in crp/db/db mice and there was a trend towards lower trabecular BV/TV in db/db and crp/db/db mice. Otherwise, cortical and trabecular bone density and microarchitecture at the proximal tibia was maintained in type 2 DM mice. Three-point bending test showed significantly lower elastic modulus and comparable loading and energy in type 2 DM mice.
Leptin receptor knock-out type 2 DM mice did not exhibit phenotype, on a bone microarchitectural level, typical of osteoporosis. Despite a large body of clinical and epidemiological studies linking type 2 DM to increased bone fragility and fracture risk, patients with type 2 DM are often found to have higher or normal BMD. Studies investigating bone microarchitecture in animal models of type 2 DM yield conflicting results24,25,26,27,28,29,30. The high bone mass phenotype at L5 in db/db mice found in our study is in consistent with the study by Ducy et al.24. They showed significantly higher trabecular BV/TV at L5 and femur in 6-month-old db/db mice. This high bone mass phenotype was found in both genders, despite coexisting hypogonadism and hypercortisolism and the appearance of this phenotype preceded the onset of obesity24. Higher trabecular bone mass at the spine (L2–3) has also been reported in a leptin-deficient (ob/ob) mice model27.
In contrast, a number of studies have reported significantly lower bone mass and/or compromised trabecular microarchitecture in db/db25,28,30 or ob/ob mice model25,27, or obese Zucker (fa/fa) rats model26,29, which is a type 2 DM model with an inactivating mutation of the leptin receptor. However, the majority of this low bone mass phenotype was found at the limbs (femur or tibia)25,26,27,28,29 whilst the bone mass at the spine was reported to be normal25 or higher27. In the study by Williams et al., although bone mass reduction was found at both the tibia and spine in db/db mice, the magnitude of the decrease was less in the spine evidenced by the finding that significant deterioration of trabecular compartment at L5 was only found in Tb.Th30. Our findings are consistent with these previous results in that we found trends towards lower trabecular bone mass and Tb.Th at the tibia in db/db mice despite the high bone mass phenotype at the L5. Additionally, bone material property at the femur was also affected in db/db mice, evidenced by a lower elastic modulus. These findings suggest that leptin- or leptin receptor-deficiency produces differing bone phenotypes at the spine and limb. The greater loss of bone at the limb than at the spine could be due to the greater muscle loss at the limb as a result of obesity27. Bone remodeling is significantly affected by the muscle because muscle contraction produces the greatest load on bone31,32 and because muscle mass is the primary determinant of blood flow to the limb33,34. In ob/ob mice, the low bone mass at the femur was associated with the relatively low hind limb muscle mass. In addition, Hamrick et al. proposed that the difference in bone phenotype between the femur and lumbar spine of ob/ob mice could be partly explained by the differing response of marrow cells at these two skeletal sites to leptin deficiency27. Leptin deficiency and obesity are known to be associated with increased bone marrow adipogenesis which has been link to bone loss35,36. Marked adiposity in the femur suggesting excessive bone marrow adipogenesis, along with an absence of increased adipocyte number in the lumbar vertebrae, has been reported in ob/ob mice27.
CRP is a measure of chronic inflammation and is an independent risk factor for type 2 DM and cardiovascular disease37. Elevated CRP level can also interact with other risk factors to accelerate the progression of type 2 DM and its related complications, particularly cardiovascular diseases37,38. Previous studies have also found significant correlation between elevated CRP level and increased risk of fracture in general population and this correlation is independent of areal BMD measured by DXA14,15,16,17. In this study, we included groups of human CRP transgenic mice to investigate the role of CRP in the development of osteoporosis in type 2 DM. Although crp/db/db mice had shorter femur length than db/db mice, overall, crp/db/db mice did not exhibit poorer bone density and architecture than db/db mice. These findings do not support that CRP plays a detrimental role in deteriorating bone density and architecture in type 2 DM. However, our study did not examine degree of mineralization or potential micro-damage to bone matrix or properties of non-mineral phase of the bone, on which CRP might have a direct or indirect effect. The exact mechanism how CRP disturb bone metabolism and induces bone fragility in general population or in type 2 DM requires further studies.
There are some limitations of this study. First, due to the difficulty of measuring the femoral neck of mice, we performed the micro-CT scanning on the L5 and the proximal tibia instead. Our results may not be applicable to the femur which is a major site for fracture in type 2 DM. Second, we did not perform assessments on bone turnover markers by blood sample or bone histomorphometry. The underlying alteration in the balance of bone metabolism responsible for the observed bone phenotype in this animal model was not studied. Finally, assessment of bone quality was conducted only at bone microarchitectural level. Some features of bone microarchitecture such as cortical porosity, micro-crack of one matrix or properties of non-mineral phase of the bone were not be able examined due to limitation of the assessment technology used for the current study. However, mechanical test was conducted to assess the whole bone strength and the results did not show significantly reduced bone strength in db/db mice.
Due to above mentioned study limitations, further studies are recommended. First of all since this study aimed to validate the secondary osteoporotic animal model, the mechanistic studies on how leptin receptor knock-out would induce increase of body weight would be subject to explore. Since we all know that leptin plays an important role in not only the contribution of type 2 DM but also bone metabolism, how this mutation would affect the bone quality would also be of our interests apart from weight bearing that is a known factor preventing bone loss. Moreover, as mentioned in results, the mineral phase of bone was not affected by the elevation of CRP the non-mineral phrase should be analyzed to understand the role of CRP on the bone structure.
In conclusion, the leptin receptor-deficient (db/db) mice did not exhibit significant compromised bone quality at microarchitectural level. However, deficiency in leptin signaling had differing effect on the spine and limb with high bone mass phenotype being particularly noticeable at the spine. There were trends towards lower trabecular bone mass and compromised microarchitecture at the tibia in the db/db mice. Overall, this mouse model does not exhibit phenotype typical of secondary osteoporosis. Human CRP transgenic db/db mice did not exhibit poorer bone mass and microarchitecture than db/db mice, suggesting that CRP does not play a detrimental role in deteriorating bone density and architecture in type 2 DM.
Ethics Approval.
The study was cond.ucted with the approval from the Animal Experimentation Ethics Committee of the Chinese University of Hong Kong (AEEC No. 09/027/MIS).
Additional Information
How to cite this article: Huang, L. et al. Validity of leptin receptor-deficiency (db/db) type 2 diabetes mellitus mice as a model of secondary osteoporosis. Sci. Rep. 6, 27745; doi: 10.1038/srep27745 (2016).
References
Ziolkowska, H., Brzewski, M. & Roszkowska-Blaim, M. Determinants of the intima-media thickness in children and adolescents with chronic kidney disease. Pediatr. Nephrol. 23, 805–811 (2008).
Janghorbani, M., Van Dam, R. M., Willett, W. C. & Hu, F. B. Systematic review of type 1 and type 2 diabetes mellitus and risk of fracture. Am. J. Epidemiol. 166, 495–505 (2007).
Barrett-Connor, E. & Holbrook, T. L. Sex differences in osteoporosis in older adults with non-insulin-dependent diabetes mellitus. JAMA 268, 3333–3337 (1992).
Strotmeyer, E. S. et al. Diabetes is associated independently of body composition with BMD and bone volume in older white and black men and women: The Health, Aging and Body Composition Study. J. Bone Miner. Res. 19, 1084–1091 (2004).
van Daele, P. L. et al. Bone density in non-insulin-dependent diabetes mellitus. The Rotterdam Study. Ann. Intern. Med. 122, 409–414 (1995).
Melton, L. J., 3rd et al. A bone structural basis for fracture risk in diabetes. J. Clin. Endocrinol. Metab. 93, 4804–4809 (2008).
Burghardt, A. J. et al. High-resolution peripheral quantitative computed tomographic imaging of cortical and trabecular bone microarchitecture in patients with type 2 diabetes mellitus. J. Clin. Endocrinol. Metab. 95, 5045–5055 (2010).
Hamann, C., Kirschner, S., Gunther, K. P. & Hofbauer, L. C. Bone, sweet bone–osteoporotic fractures in diabetes mellitus. Nature reviews. Endocrinology 8, 297–305 (2012).
Hein, G. E. Glycation endproducts in osteoporosis–is there a pathophysiologic importance? Clin. Chim. Acta 371, 32–36 (2006).
Saito, M., Fujii, K., Mori, Y. & Marumo, K. Role of collagen enzymatic and glycation induced cross-links as a determinant of bone quality in spontaneously diabetic WBN/Kob rats. Osteoporos. Int. 17, 1514–1523 (2006).
Schwartz, A. V. et al. Pentosidine and increased fracture risk in older adults with type 2 diabetes. J. Clin. Endocrinol. Metab. 94, 2380–2386 (2009).
Rosen, C. J. & Klibanski, A. Bone, fat and body composition: evolving concepts in the pathogenesis of osteoporosis. Am. J. Med. 122, 409–414 (2009).
Fujii, H., Hamada, Y. & Fukagawa, M. Bone formation in spontaneously diabetic Torii-newly established model of non-obese type 2 diabetes rats. Bone 42, 372–379 (2008).
Pasco, J. A. et al. High-sensitivity C-reactive protein and fracture risk in elderly women. JAMA 296, 1353–1355 (2006).
Schett, G. et al. High-sensitivity C-reactive protein and risk of nontraumatic fractures in the Bruneck study. Arch. Intern. Med. 166, 2495–2501 (2006).
Nakamura, K. et al. C-reactive protein predicts incident fracture in community-dwelling elderly Japanese women: the Muramatsu study. Osteoporos. Int. 22, 2145–2150 (2011).
Eriksson, A. L. et al. High-sensitivity CRP is an independent risk factor for all fractures and vertebral fractures in elderly men: the MrOS Sweden study. J. Bone Miner. Res. 29, 418–423 (2014).
King, D. E., Mainous, A. G., 3rd, Buchanan, T. A. & Pearson, W. S. C-reactive protein and glycemic control in adults with diabetes. Diabetes Care 26, 1535–1539 (2003).
Mugabo, Y., Li, L. & Renier, G. The connection between C-reactive protein (CRP) and diabetic vasculopathy. Focus on preclinical findings. Current diabetes reviews 6, 27–34 (2010).
Ziegler, D. Type 2 diabetes as an inflammatory cardiovascular disorder. Current molecular medicine 5, 309–322 (2005).
Chen, H. et al. Evidence that the diabetes gene encodes the leptin receptor: identification of a mutation in the leptin receptor gene in db/db mice. Cell 84, 491–495 (1996).
Hildebrand, T. & Ruegsegger, P. Quantification of Bone Microarchitecture with the Structure Model Index. Comput Methods Biomech Biomed Engin 1, 15–23 (1997).
He, Y. X. et al. Impaired bone healing pattern in mice with ovariectomy-induced osteoporosis: A drill-hole defect model. Bone 48, 1388–1400 (2011).
Ducy, P. et al. Leptin inhibits bone formation through a hypothalamic relay: a central control of bone mass. Cell 100, 197–207 (2000).
Ealey, K. N., Fonseca, D., Archer, M. C. & Ward, W. E. Bone abnormalities in adolescent leptin-deficient mice. Regul. Pept. 136, 9–13 (2006).
Hamann, C. et al. Delayed bone regeneration and low bone mass in a rat model of insulin-resistant type 2 diabetes mellitus is due to impaired osteoblast function. American journal of physiology. Endocrinology and metabolism 301, E1220–1228 (2011).
Hamrick, M. W., Pennington, C., Newton, D., Xie, D. & Isales, C. Leptin deficiency produces contrasting phenotypes in bones of the limb and spine. Bone 34, 376–383 (2004).
Lorentzon, R., Alehagen, U. & Boquist, L. Osteopenia in mice with genetic diabetes. Diabetes Res. Clin. Pract. 2, 157–163 (1986).
Tamasi, J. A., Arey, B. J., Bertolini, D. R. & Feyen, J. H. Characterization of bone structure in leptin receptor-deficient Zucker (fa/fa) rats. J. Bone Miner. Res. 18, 1605–1611 (2003).
Williams, G. A. et al. Skeletal phenotype of the leptin receptor-deficient db/db mouse. J. Bone Miner. Res. 26, 1698–1709 (2011).
Burr, D. B. Muscle strength, bone mass and age-related bone loss. J. Bone Miner. Res. 12, 1547–1551 (1997).
Frost, H. M. On our age-related bone loss: insights from a new paradigm. J. Bone Miner. Res. 12, 1539–1546 (1997).
Dinenno, F. A., Seals, D. R., DeSouza, C. A. & Tanaka, H. Age-related decreases in basal limb blood flow in humans: time course, determinants and habitual exercise effects. The Journal of physiology 531, 573–579 (2001).
Raitakari, M. et al. Relationship between limb and muscle blood flow in man. The Journal of physiology 496(Pt 2), 543–549 (1996).
Thomas, T. et al. Leptin acts on human marrow stromal cells to enhance differentiation to osteoblasts and to inhibit differentiation to adipocytes. Endocrinology 140, 1630–1638 (1999).
Justesen, J. et al. Adipocyte tissue volume in bone marrow is increased with aging and in patients with osteoporosis. Biogerontology 2, 165–171 (2001).
Kimberly, M. M., Cooper, G. R. & Myers, G. L. An overview of inflammatory markers in type 2 diabetes from the perspective of the clinical chemist. Diabetes technology & therapeutics 8, 37–44 (2006).
Pfutzner, A. & Forst, T. High-sensitivity C-reactive protein as cardiovascular risk marker in patients with diabetes mellitus. Diabetes technology & therapeutics 8, 28–36 (2006).
Acknowledgements
Major State Basic Research Development Program of People’s Republic of China (grant number. 2012CB51770). Shenzhen Basic Research Program (SZSITC) of People’s Republic of China [grant number. JC201104220290A]. Collaborative Research Funding of Hong Kong Special Administrative Region (Ref. No.:CUHK5/CRF/09)
Author information
Authors and Affiliations
Contributions
All authors were responsible for study design, the collection, analysis and interpretation of all data, the writing of the article and the decision to publish. Then transgenic mice model was handled by Y.-k.Y., X.-r. H. and H.-y.C. Sample collection and assessments were done by L.H., L.-z.Z. and D.Y. Study design, data analysis and interpretation were handle by L.H. Drafting the manuscript was done by L.H. and T.Y.Z.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Huang, L., You, Yk., Zhu, T. et al. Validity of leptin receptor-deficiency (db/db) type 2 diabetes mellitus mice as a model of secondary osteoporosis. Sci Rep 6, 27745 (2016). https://doi.org/10.1038/srep27745
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep27745
This article is cited by
-
Exercise improves bone formation by upregulating the Wnt3a/β-catenin signalling pathway in type 2 diabetic mice
Diabetology & Metabolic Syndrome (2021)
-
Intervertebral disc degeneration in mice with type II diabetes induced by leptin receptor deficiency
BMC Musculoskeletal Disorders (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.