Abstract
Objective
Whether and under what circumstances medical residents seek personal health care is a growing concern that has important implications for medical education and patient welfare, but has not been thoroughly investigated. Barriers to obtaining care have been previously documented, but very little empirical work has focused on trainees who seek health care at their home institution.
Methods
A self-report survey on special issues in personal health care of residents was created and distributed at the University of New Mexico School of Medicine in 2001. The authors report findings regarding stigma, fear of jeopardy to training status, and attitudes toward seeking self-care for residents in dual roles as patients and trainees.
Results
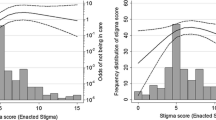
Residents (N = 155) rated their concerns regarding stigma and jeopardy to training status and the likelihood of seeking care at their training institution for six vignettes. The vignettes were paired to make comparisons between attending or supervisor as treating physician and between clinical scenarios. Alcohol abuse, nausea and diarrhea, panic attacks, and pregnancy were the most highly stigmatizing to residents; diabetes and hypertension were the least. Differences were also found for gender and specialty.
Conclusion
Residents’ perceived stigma for clinical situations was an influential factor, strongly affecting concern about jeopardizing training status and likelihood of avoiding care at their home institution.
Similar content being viewed by others
References
Thomas MR, Dyrbye LN, Huntington JL, et al: How do distress and well-being relate to medical student empathy? A multicenter study. J Gen Intern Med 2007; 22: 177–183
West CP, Huschka MM, Novotny PJ, et al: Association of perceived medical errors with resident distress and empathy: a prospective longitudinal study. JAMA 2006; 296: 1071–1078
Schwartz C, Meisenhelder JB, Ma Y, et al: Altruistic social interest behaviors are associated with better mental health. Psychosom Med 2003; 65: 778–785
Boisaubin EV, Levine RE: Identifying and assisting the impaired physician. Am J Med Sci 2001; 322: 31–36
Firth-Cozens J: Interventions to improve physicians’ well-being and patient care. Soc Sci Med 2001; 52: 215–222
Dyrbye LN, Thomas MR, Shanafelt TD: Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med 2006; 81: 354–373
Stack S: Suicide risk among physicians: a multivariate analysis. Arch Suicide Res 2004; 8: 287–292
Schernhammer ES, Colditz GA: Suicide rates among physicians: a quantitative and gender assessment (meta-analysis). Am J Psychiatry 2004; 161: 2295–2302
Gundersen L: Physician burnout. Ann Intern Med 2001; 135: 145–148
Frank E, Biola H, Burnett CA: Mortality rates and causes among U.S. physicians. Am J Prev Med 2000; 19: 155–159
Deckard G, Meterko M, Field D: Physician burnout: an examination of personal, professional, and organizational relationships. Med Care 1994; 32: 745–754
Young EH: Health promoting behaviors of family practice residents: do they compare with the general public? Fam Med 1988; 20: 437–442
Lewis CE, Clancy C, Leake B, et al: The counseling practices of internists. Ann Intern Med 1991; 114: 54–58
Schwartz JS, Lewis CE, Clancy C, et al: Internists’ practices in health promotion and disease prevention: a survey. Ann Intern Med 1991; 114: 46–53
Gross CP, Mead LA, Ford DE, et al: Physician, heal thyself? Regular source of care and use of preventive health services among physicians. Arch Intern Med 2000; 160: 3209–3214
Campbell S, Delva D: Physician do not heal thyself: survey of personal health practices among medical residents. Can Fam Physician 2003; 49: 1121–1127
Davidson SK, Schattner PL: Doctors’ health-seeking behavior: a questionnaire survey. Med J Aust 2003; 179: 302–305
Rosen IM, Christie JD, Bellini LM, et al: Health and health care among house staff in four U.S. internal medicine residency programs. J Gen Intern Med 2000; 15: 116–121
Baldwin PJ, Dodd M, Wrate RM: Young doctors’ health-II. Health and health behavior. Soc Sci Med 1997; 45: 41–44
McKevitt C, Morgan M, Dundas R, et al: Sickness absence andworking through’ illness: a comparison of two professional groups. J Public Health Med 1997; 19: 295–300
Tyssen R, Vaglum P, Gronvold NT, et al: Factors in medical school that predict postgraduate mental health problems in need of treatment: a nationwide and longitudinal study. Med Educ 2001; 35: 110–120
Brimstone R, Thistlethwaite JE, Quirk F: Behavior of medical students in seeking mental and physical health care: exploration and comparison with psychology students. Med Educ 2007; 41: 74–83
Hooper C, Meakin R, Jones M: Where students go when they are ill: how medical students access health care. Med Educ 2005; 39: 588–593
Tyssen R, Rovik JO, Vaglum P, et al: Help-seeking for mental health problems among young physicians: is it the most ill that seeks help? A longitudinal and nationwide study. Soc Psychiatry Psychiatr Epidemiol 2004; 39: 989–993
Roberts LW, Warner TD, Trumpower D: Medical students’ evolving perspectives on their personal health care: clinical and educational implications of a longitudinal study. Compr Psychiatry 2000; 41: 303–314
Louie AK, Roberts LW, Coverdale J: The enculturation of medical students and residents. Acad Psychiatry 2007; 31: 253–257
Haidet P, Stein HF: The role of the student-teacher relationship in the formation of physicians: the hidden curriculum as process. J Gen Intern Med 2006; 21(suppl 1): S16–S20
Klitzman R: “Post-residency disease” and the medical self: identity, work, and health care among doctors who become patients. Perspect Biol Med 2006; 49: 542–552
Friedland AR, Farber NJ, Collier VU: Health care provided by program directors to their resident physicians and families. J Gen Intern Med 2006; 21: 1310–1312
Dunn LB, Moutier CY, Green Hammond KA, et al: Personal health care of residents: preferences for care outside of the training institution. Acad Psychiatry 2008; 32: 20–30
Pitt E, Rosenthal MM, Gay TL, et al: Mental health services for residents: more important than ever. Acad Med 2004; 79: 840–844
Roeloffs C, Sherbourne C, Unutzer J, et al: Stigma and depression among primary care patients. Gen Hosp Psychiatry 2003; 25: 311–315
Mann CE, Himelein MJ: Factors associated with stigmatization of persons with mental illness. Psychiatr Serv 2004; 55: 185–187
Ahern J, Stuber J, Galea S: Stigma, discrimination and the health of illicit drug users. Drug Alcohol Depend 2007; 88: 188–196
Feifel D, Moutier CY, Swerdlow NR: Attitudes toward psychiatry as a prospective career among students entering medical school. Am J Psychiatry 1999; 156: 1397–1402
Henry RC, Wright DE: When do medical students become human subjects of research? The case of program evaluation. Acad Med 2001; 76: 871–875
Tolich M, Baldwin KM: Unequal protection for patient rights: the divide between university and health ethics committees. J Bioeth Inq 2005; 2: 34–40
Chew-Graham CA, Rogers A, Yassin N: ‘I wouldn’t want it on my CV or their records’: medical students’ experiences of help-seeking for mental health problems. Med Educ 2003; 37: 873–880
Bragger JD, Kutcher E, Morgan J, et al: The effects of the structured interview on reducing biases against pregnant job applicants. Sex Roles 2002; 46: 215–226
Cotter DA, Hermsen JM, Ovadia S, et al: The glass ceiling effect. Soc Forces 2001; 80: 655–681
Lyness KS, Thompson CA, Francesco AM, et al: Work and pregnancy: individual and organizational factors influencing organizational commitment, timing of maternity leave, and return to work. Sex Roles 1999; 41: 485–508
Roberts LW, Warner TD, Carter D, et al: Caring for medical students as patients: access to services and care-seeking practices of 1,027 students at nine medical schools. Collaborative Research Group on Medical Student Healthcare. Acad Med 2000; 75: 272–277
Roberts LW, Warner TD, Lyketsos C, et al: Perceptions of academic vulnerability associated with personal illness: a study of 1,027 students at nine medical schools. Collaborative Research Group on Medical Student Healthcare. Compr Psychiatry 2001; 42: 1–15
Fogel SP, Sneed JR, Roose SP: Survey of psychiatric treatment among psychiatric residents in Manhattan: evidence of stigma. J Clin Psychiatry 2006; 67: 1591–1598
Dabrow S, Russell S, Ackley K, et al: Combating the stress of residency: one school’s approach. Acad Med 2006; 81: 436–439
Author information
Authors and Affiliations
Corresponding author
Additional information
Drs. Moutier, Cornette, Lehrmann, Geppert, and Green Hammond and Ms. DeBoard declared no competing interests. Dr. Laura Roberts’ work is funded through the Research for a Healthier Tomorrow-Program Development Fund, a component of the Advancing a Healthier Wisconsin endowment at the Medical College of Wisconsin. Disclosures of Academic Psychiatry editors are published in each January issue. Manuscripts authored by an editor of Academic Psychiatry or by a member of its editorial board undergo the same editorial review process, including blinded peer review, applied to all manuscripts. Additionally, the Editor is recused from any editorial decision-making.
Rights and permissions
About this article
Cite this article
Moutier, C., Cornette, M., Lehrmann, J. et al. When Residents Need Health Care: Stigma of the Patient Role. Acad Psychiatry 33, 431–441 (2009). https://doi.org/10.1176/appi.ap.33.6.431
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1176/appi.ap.33.6.431