Abstract
Background
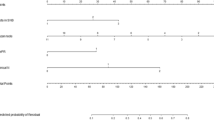
With increasing frequency, breast cancer patients and clinicians are questioning the need for completion axillary lymph node dissection (ALND) in the setting of a positive sentinel lymph node (SLN). We previously developed a nomogram to estimate the likelihood of residual disease in the axilla after a positive SLN biopsy result. In this study, we compared the predictions of clinical experts with those generated by the nomogram and evaluated the ability of the nomogram to change clinicians’ behavior.
Methods
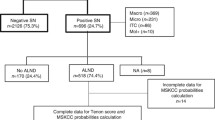
Pathologic features of the primary tumor and SLN metastases of 33 patients who underwent completion ALND were presented to 17 breast cancer specialists. Their predictions for each patient were recorded and compared with results from our nomogram. Subsequently, clinicians were presented with clinical information for eight patients and asked whether they would perform a completion ALND before and after being presented with the nomogram prediction.
Results
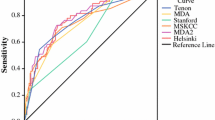
The predictive model achieved an area under the receiver operating characteristic curve of .72 when applied to the test data set of 33 patients. In comparison, the clinicians as a group were associated with an area under the receiver operating characteristic curve of .54 (P < .01 vs. nomogram). With regard to performing a completion ALND, providing nomogram results did not alter surgical planning.
Conclusions
Our predictive model seemed to substantially outperform clinical experts. Despite this, clinicians were unlikely to change their surgical plan based on nomogram results. It seems that most clinicians can improve their predictive ability by using the nomogram to predict the likelihood of additional non-SLN metastases in a woman with a positive SLN biopsy result.



Similar content being viewed by others
References
Hunink M, Glasziou P. Decision Making in Health and Medicine: Integrating Evidence and Values. Cambridge, UK: Cambridge University Press, 2001
Weisstein EW. Nomogram. In: MathWorld—A Wolfram Web Resource. Available at: http://mathworld.wolfram.com/Nomogram.html
Van Zee KJ, Manasseh DE, Bevilacqua JB, et al. A nomogram for predicting the likelihood of additional nodal metastases in breast cancer patients with a positive sentinel node biopsy. Ann Surg Oncol 2003;10:1140–51
Temple LKF, Baron R, Cody HS III, et al. Sensory morbidity after sentinel lymph node biopsy and axillary dissection: significant and persistent sequelae. Ann Surg Oncol 2002;9:654–62
Pepe M. The Statistical Evaluation of Medical Tests for Classification and Prediction. Oxford: Oxford University Press, 2003
SAS/STAT User Manual. Version 9. Cary, NC: SAS Institute, 2003
Obuchowski NA. On the comparison of correlated proportions for clustered data. Stat Med 1998;17:1495–507
Ross PL, Gerigk C, Gonen M, et al. Comparisons of nomograms and urologists’ predictions in prostate cancer. Semin Urol Oncol 2002;20:82–8
Ross PL, Scardino PT, Kattan MW. A catalog of prostate cancer nomograms. J Urol 2001;165:1562–8
Author information
Authors and Affiliations
Corresponding author
Additional information
Published by Springer Science+Business Media, Inc. © 2005 The Society of Surgical
Oncology, Inc.
Rights and permissions
About this article
Cite this article
Specht, M.C., Kattan, M.W., Gonen, M. et al. Predicting Nonsentinel Node Status After Positive Sentinel Lymph Biopsy for Breast Cancer: Clinicians Versus Nomogram. Ann Surg Oncol 12, 654–659 (2005). https://doi.org/10.1245/ASO.2005.06.037
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/ASO.2005.06.037