Abstract
Background: Aggressive surgical resection of neuroendocrine tumour liver metastases (NET-LM) is associated with symptomatic relief. Debulking up to 90% of tumour burden, even with positive margins, may be beneficial. However, patients with diffuse hepatic metastases may not qualify for resection owing to associated insufficient remnant liver parenchyma. The purpose of this study is to describe an early experience with a hepatic parenchymal preserving (HPP) approach.
Methods: We retrospectively reviewed our institutional neuroendocrine tumours database to identify patients with NET-LM, including symptomatic patients with extensive bilobar involvement, who underwent virtual volumetric assessment (VVA) combined with HPP resection between October 2008 and July 2011.
Results: Our study involved 9 patients. The median number of liver metastases resected was 10 (range 4–50). Symptomatic improvement was observed in all patients. Immediate postoperative normalization of 5-HIAA 24-hour urine levels occurred in 89% of patients. Symptomatic and biochemical response remained stable or improved in 75% of patients at 12 months of follow-up. Four patients had postoperative complications. There was no 90-day mortality.
Conclusion: The described HPP approach is feasible and safe. Most patients experienced symptomatic and biochemical improvement. This reproducible approach could expand surgical resection options for patients with NET-LM and diffuse bilobar involvement.
Neuroendocrine tumours (NET) represent a diverse set of cancers with heterogeneous behaviour. Metastatic disease at presentation is documented in 30%–90% of patients, occurring more frequently in those with pancreatic and intestinal NET.1 Neuroendocrine tumours of gastrointestinal origin often metastasize to the liver and can be symptomatic as a result of carcinoid syndrome. Although they are often thought of as slow-growing tumours, once they have metastasized to the liver, if untreated, they have a 30%–40% 5-year survival.2
Systemic chemotherapy has been generally ineffective in the treatment of neuroendocrine liver metastases of non-pancreatic origin.3 However, for unresectable or metastatic pancreatic NET, directed therapies, such as everolimus, an m-TOR inhibitor, and sunitinib, a tyrosine kinase inhibitor, have been found to increase progression-free survival.4,5 The effect of these agents in NET of nonpancreatic origin has yet to be demonstrated. Somatostatin receptor analogues (SSAs) are also beneficial for the treatment of patients with metastatic disease, but do not provide long-lasting benefits in all patients.6 In addition, the main benefit from SSAs in delaying tumour progression occurs in patients with less than 10% liver replacement.7 Surgical resection combined with SSA for symptomatic control has been the mainstay of treatment for neuroendocrine tumour liver metastases (NET-LM) when feasible.
Given the rarity of the disease and its slow progression, there has been controversy and lack of a standard definition for the potential and optimal surgical treatments available. Surgical management for NET-LM can be divided into potentially curative or palliative resections based on the burden of disease. Potential curative intent refers to a complete resection of all gross disease confined to the liver with microscopically negative margins (R0). Curative resections have generally been accomplished with resection of the primary, lymphadenectomy, formal anatomic liver resections and/or nonanatomic wedge resections.8,9 The resections may also be performed with transarterial embolization (TAE), transarterial chemoembolization (TACE) or radiofrequency ablation (RFA) as adjuncts.10,11 The latest European Neuroendocrine Tumor Society (ENETS) Consensus Guidelines support the use of such resections for metastatic disease confined to a single lobe or adjacent segments, or in cases where a single lobe is the location of the majority of the tumour burden with smaller sites of disease involving the other lobe.10 However, the guidelines also state that diffuse, multifocal liver metastases should not be treated surgically with curative intent. In addition, although improved survival has been demonstrated when resections have been completed with a curative intent, up to 75% of the patients will have a recurrence at 5 years.12
The palliative approach refers to debulking for symptom and/or tumour control, with at least 90% of the tumour burden being removed in order to achieve this goal, according to some authors.13 Palliative resections, like resections for curative intent, have consisted of anatomic or nonanatomic resections in an effort to remove as much gross disease as possible. There is lack of consensus as to the timing and extent of surgery that should be undertaken and to what outcome. Symptomatic relief has been accepted as a reasonable goal of surgical intervention, but this approach is limited in some patients who have extensive liver involvement.
The aim of this study was to describe our early experience with a hepatic parenchymal preserving (HPP) approach that could expand surgical resection options for symptomatic patients with NET-LM and diffuse bilobar involvement.
Methods
We performed a retrospective review of the prospectively collected Sunnybrook Health Sciences Centre’s neuroendocrine tumours database to identify patients with NET-LM who underwent an HPP approach between October 2008 and July 2011. We reviewed their electronic medical records, imaging reports, pathology reports and clinic notes. Data were collected pertaining to patient demographic characteristics, site of the primary tumour, pathology, symptoms, chromogranin A (CgA) and 5-hydroxyindoleacetic acid (5-HIAA) 24-hour urine levels, number and size of hepatic metastases, operative management and perioperative morbidity and mortality.
Consideration for the HPP approach was given to symptomatic patients with extensive bilobar hepatic metastases. The intent of the surgical intervention in all patients was palliative. The extent of resection was determined based on preoperative magnetic resonance imaging (MRI) or computed tomography (CT), intraoperative clinical assessment and/or intraoperative ultrasonography. The goal was to remove at least 90% of the liver tumour burden, based on preoperative imaging modalities, in order to achieve symptomatic improvement.
The preoperative workup for all patients included a focused history and physical examination, blood work, including CgA, 5-HIAA 24-hour urine levels, and CT or MRI of the chest, abdomen and pelvis. At our institution, it is not routine practice to evaluate patients with octreotide scans. Data pertaining to preoperative assessment were also collected in a retrospective manner.
Patients were selected for the HPP approach if they were symptomatic secondary to diffuse, bilobar liver metastases and if they were not candidates for standard resections. In accordance with the ENETS Consensus Guidelines, patients with liver metastases confined to 1 lobe or adjacent segments underwent standard anatomic resections. Similarly, patients with either 1 lobe primarily affected but with contralateral or deep satellite lesions were considered for TAE, with or without anatomic resection(s). Radiofrequency ablation was not used in this patient population given the large burden of disease that would necessitate repeated treatments, with treatments limited by tumour size and proximity to vital structures.8
Our proposed approach encompassed HPP resections in combination with perioperative virtual volumetric assessment (VVA). The HPP procedure consisted of multiple enucleations for lesions in the liver parenchyma combined with wedge resections and nonanatomic and anatomic resections in order to remove at least 90% of the disease burden while simultaneously sparing a remnant liver parenchyma of greater than 30%. We used a technique that involved the identification of a peritumoural plane in which direct blood vessels and parenchyma adherent to the tumour were ligated with the application of a collagen sealing device, resulting in complete, gross enucleation with maximal preservation of the surrounding parenchyma. By identifying a peritumoural plane, the lesions were separated and extracted from the adjacent parenchyma. This allowed the surrounding parenchyma to remain relatively intact, such that both superficial and deep lesions could be accessed and resected with minimal surrounding trauma. The identification of deep lesions was guided by intraoperative ultrasonography. Retrospectively, VVA was performed on patients’ CT scans or MRIs by a single radiologist (L.M.). The segmentation was performed using the GE workstation volumeshare 2 (GE Healthcare). Multiple techniques of segmentation were applied. First, liver contours were drawn on the 3-dimensional volume and segmented. The value of the total liver volume, including metastases, was saved and recorded. Then, a threshold technique was performed on the liver volume obtained, allowing the segmentation of the tumours from the liver parenchyma. If available, MRI was preferred for the segmentation due to the higher lesion to parenchyma contrast ratio. A threshold technique was favoured over a manual segmentation of the metastases because the lesions were too numerous and were located diffusely throughout the liver parenchyma. The distribution and characteristics of the lesions did not allow the radiologist to perform a classic standardized future liver remnant volumetric analysis. At the end of the process, the volume of the liver, excluding the metastases, was obtained. To ensure accuracy, reverse processing was performed to assess the tumour volume. The ratio of total liver volume minus metastases over total liver volume yielded estimates of preoperative parenchymal preservation expected with the HPP procedure. Similar measurements were performed on postoperative imaging to determine residual disease and remaining liver parenchyma. The overall process required approximately 20 minutes per patient to complete.
The study was approved by the Sunnybrook Health Sciences Centre Review Ethics Board.
Results
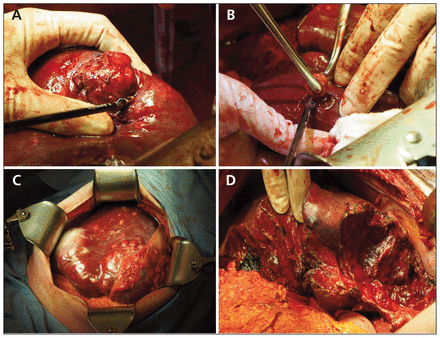
We identified 9 patients who underwent HPP during our study period: 5 women and 4 men. Patient demographics, tumour and resection characteristics and outcomes are described in Table 1. The HPP approach is shown in Figures 1 and 2.
Hepatic parenchymal preserving (HPP) technique for resection of neuroendocrine tumour liver metastases. (A, B) Identification of a peritumoural plane and enucleation of metastases. (C) Preresection appearance of the liver. (D) Liver appearance following HPP resection.
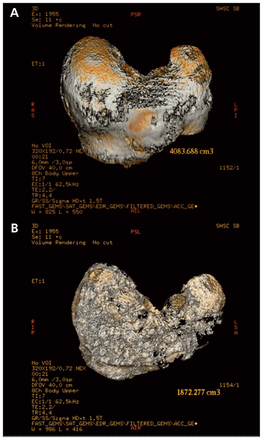
Virtual volumetric assessment for perioperative assessment of tumour burden of neuroendocrine tumour liver metastases. (A) Preoperative total liver volume. (B) Preoperative tumour volume isolated.
Patient demographic characteristics, characteristics of primary tumour and liver metastases, perioperative management and findings, and postoperative outcomes of patients undergoing the hepatic parenchymal preserving approach for neuroendocrine tumour liver metastases
Symptomatic response
Symptoms were subjectively reported based on detailed questioning of patients at preoperative and follow-up appointments. All patients reported being symptomatic preoperatively and were not experiencing a response to increasing SSA doses. Seven patients reported experiencing flushing, 8 patients had diarrhea, 3 patients experienced cramping or abdominal pain and 1 patient reported fatigue. Four patients described complete resolution of all their symptoms, and the remaining 5 patients reported overall improvement in their symptoms following surgery. At 6-and 12-month follow-up intervals, 6 of 8 patients reported improvement or stability in their symptoms.
Biochemical response
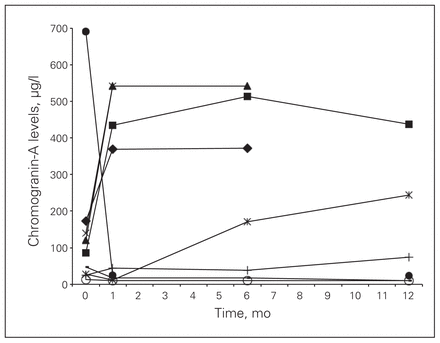
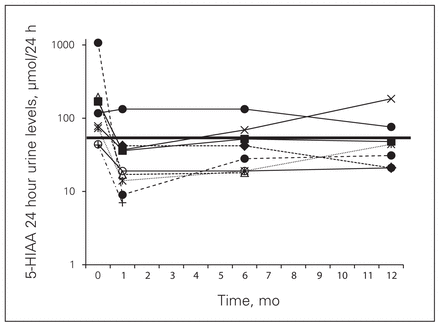
All patients had CgA levels and 8 patients had 5-HIAA 24-hour urine levels measured preoperatively. Perioperative CgA and 5-HIAA 24-hour urine levels are shown in Figures 3 and 4.
Postoperative chromogranin A levels for each patient from time of surgery. The upper limit of normal is 100 μg/L.
Postoperative 5-hydroxyindoleacetic acid (5-HIAA) 24-hour urine levels for each patient from time of surgery on a logarithmic scale. The upper limit of normal is 50 μmol/24 hours (represented by dark horizontal line).
Virtual volumetric assessment
Retrospective VVA performed on preoperative imaging revealed up to 35.7% liver replacement, with a median of 8.4% (range 0.8%–35.7%) of the total liver volume replaced by metastatic disease. All patients who had perioperative imaging and were amenable to VVA (9 patients) had at least 72.5% parenchymal preservation. The median preoperative to postoperative parenchymal preservation was 103.3% (range 72.5%–154.6%). Six of the patients with complete parenchymal preservation had a greater volume of liver parenchyma postoperatively. On postoperative VVA, only 2 patients had residual disease, while 7 patients had no detectable disease on imaging.
Outcomes
Operative complications were observed in 4 patients and included 4 intra-abdominal collections managed successfully with percutaneous drainage. Two of the patients with collections presented after discharge and required readmission for 2–3 days to facilitate drain placement. Other complications included a urinary tract infection and Clostridium difficile infection. According to the Clavien–Dindo classification of surgical complications,14 there were 4 grade IIIa and 2 grade II complications.
Discussion
Patients with carcinoid syndrome as a result of neuroendocrine tumour liver metastases can be debilitated by the resultant flushing, diarrhea or abdominal pain.15 Debulking up to 90% of tumour burden, even with positive margins, has been shown to be beneficial for symptom relief.6
In the present study, 9 patients were identified who did not meet criteria for standard resections owing to the diffuse nature of their liver metastases but who were increasingly symptomatic, despite systemic therapies, secondary to their disease burden. While standard resections may be beneficial in debulking some of their disease, it would have been unlikely to meet a target of removing at least 90% of the liver metastases while preserving an adequate amount of normal liver parenchyma. An HPP approach was undertaken in these patients with a primary goal of symptomatic relief. A parenchymal-sparing technique has been described previously for the management of primary pancreatic neuroendocrine tumours,16 but not in the management of neuroendocrine tumour hepatic metastases. The patients in the present study represent a highly selected group of symptomatic patients who were not candidates for standard anatomic liver resections and in whom ablative or embolization techniques alone would not have provided adequate symptomatic control given the extensive number of liver metastases present. The HPP approach is aimed at such patients, who represent a gap in the management strategies currently available.
Given the characteristics of HPP resections, not surprisingly, positive margins on pathologic assessment were reported for all patients. While it is necessary to obtain negative margins in curative resections of other liver metastases, such as colorectal carcinomas, the impact of margin status in NET-LM is unclear. The heterogeneous behaviour of NET in some patients may allow for potential symptomatic benefit from liver resections, even with positive margins, for diffuse multifocal liver metastases as long as sufficient liver parenchyma is preserved.
Palliative resections have been shown to be beneficial for symptomatic relief for NET-LM.17 All of the patients who underwent the HPP approach proposed here experienced improvement in their symptoms; 4 patients experienced complete resolution of their symptoms in the immediate postoperative period. Que and colleagues6 found that although symptomatic improvement was similar between resections for curative and palliative intent, patients who underwent palliative resections had earlier symptomatic recurrence. It was not unexpected that debulking procedures resulted in early symptomatic recurrence; however, in the present study longer follow-up was required to determine the mean time to symptomatic recurrence.
Biochemical markers of neuroendocrine tumours were also assessed in the present study. Chromogranin A levels were generally not improved by HPP resection, as 5 patients had elevated CgA levels postoperatively. However, CgA did not appear to correlate with symptom control. Woltering and colleagues18 found that while CgA levels may reflect tumour differentiation and tumour burden, the levels were inversely related to symptom control post-treatment. Although many patients had increased CgA levels following HPP resection, this did not appear to alter the primary outcome of symptomatic relief. Most patients with elevated 5-HIAA 24-hour urine levels measured perioperatively demonstrated normalization of their levels up to 12 months later. This suggests that, similar to standard complete resections for NET-LM, the proposed HPP approach is associated with biochemical improvement postoperatively. Given the symptomatic improvements postoperatively, it is not surprising that 5-HIAA, a breakdown product of serotonin, shows a similar improvement. Elevated 5-HIAA levels are also associated with an increased risk of carcinoid heart disease.19 Therefore, improvements in 5-HIAA levels following the HPP approach may alter the natural history of such heart disease. Longer follow-up is necessary to determine the durability of this biochemical improvement, but this technique appears promising.
Virtual volumetric assessment was described in this study as a potential adjunct to the HPP resection. Volumetrics are routinely used to calculate the amount of future liver remnant (FLR) following anatomic resections. However, standard volumetrics are not applicable for non-anatomic resections since they incorporate the amount of normal liver parenchyma that will be removed based on anatomic landmarks. While the amount of liver replacement calculated by VVA in the present study appears quite low, it would be much higher in the described patients if standard liver remnant calculations and resections had been undertaken, such that they would not have been eligible for such approaches. It appears as though there was relatively rapid hepatic growth given that several patients had an increase in their postoperative parenchymal volumes. The liver has the unique ability to regenerate following surgery or injury, with normal liver weight being obtained 8–15 days following partial hepatectomy in humans.20 However, this finding may also be attributed to differences in calculations between perioperative images or to the timing of the imaging, given the retrospective nature of the study. This imaging technique was described and used to assess the total liver volume compared with the tumour burden to provide estimates of the remaining liver parenchyma in the setting of the HPP approach. Virtual volumetric assessment appears to be a feasible approach for the assessment of patients undergoing HPP resections, but validation of the technique in the context of HPP resections needs to be undertaken. For further assessment and validation of the HPP approach, VVA could be facilitated by the use of MRI with gadolinium ethoxybenzyl dimeglumine (Bayer HealthCare Pharmaceuticals Inc.) preoperatively. In addition, Ribero and colleagues21 have described that calculations for total estimated liver volume that use body surface area provide more accurate FLR calculations.
Although the HPP approach is appropriate for patients with diffuse liver involvement, which may not be suitable for standard resections, one must still undertake the approach in a safe manner that allows resection of the majority of the tumour burden while maintaining adequate normal liver parenchyma. The HPP approach is suggested for preservation of liver parenchyma in the setting of bilobar disease that would otherwise require extensive resection of adjacent normal liver parenchyma, not for heroic measures.
Limitations
The present study is limited by its retrospective nature and small sample size. Future studies will aim to incorporate intraoperative outcome measures and objective symptomatic assessments. Despite these limitations, the results appear promising in this group of patients.
Conclusion
The described HPP approach offers symptom relief and improvement in biochemical parameters in the majority of patients studied. This is a reproducible approach that has the potential to expand surgical resection options for palliative intent for patients in whom systemic treatments or directed therapies have failed and who are increasingly symptomatic as a result of diffuse bilobar liver metastases. In addition, VVA may be used to guide selection and evaluation of such patients.
Footnotes
Previous presentation at the Canadian Society of Surgical Oncology’s Annual Scientific Meeting, Apr. 27, 2012.
Competing interests: None declared.
Contributors: All authors designed the study and analyzed the data. A. Nadler, M. Cukier and L. Milot acquired the data. A. Nadler, M. Cukier and C.H. Law wrote the article, which all authors reviewed and approved for publication.
- Accepted April 2, 2013.