Abstract
Synopsis
Zonisamide is a 1,2 benzisoxazole derivative and the first agent of this chemical class to be developed as an antiepileptic drug. It has shown activity in various animal models of epilepsy, and although a detailed mode of action awaits clarification it appears to block the propagation/spread of seizure discharges and to suppress the epileptogenic focus.
Clinical experience with zonisamide in Japan has documented its efficacy in the treatment of partial seizures (partial-onset generalised tonic-clonic, simple partial and/or complex partial seizures), and to a more variable extent, generalised tonic-clonic, generalised tonic (mainly seen in symptomatic generalised epilepsies including Lennox-Gastaut Syndrome) and compound/combination seizures (including those refractory to treatment with other antiepileptic drugs). Other generalised seizure types have also responded to therapy with zonisamide, although only small patient numbers were studied. Zonisamide has demonstrated efficacy equivalent to that of carbamazepine in patients with (mainly) partial seizures, and to that of valproic acid in a small study of children (n = 32) with generalised seizures.
Animal studies suggest that zonisamide possesses a more favourable therapeutic index than most other antiepileptic drugs. However, clinical trials conducted to date, have not confirmed any overt tolerability advantage. Indeed, whereas the recommended therapeutic plasma zonisamide concentration is 20 mg/L, clinical investigations have associated adverse events with plasma zonisamide concentrations of >30 mg/L, suggesting the usefulness of therapeutic drug monitoring. Moreover, although plasma concentrations of zonisamide are empirically regarded to be proportional to therapeutic doses in patients in Japan, nonlinear pharmacokinetics have been reported for this drug in patients in the US and may further complicate its use in this patient population. Additional pharmacokinetic studies will help to establish the change in pharmacokinetic profile that occurs with dosage titration in patients outside Japan. Among 700 patients treated with zonisamide in Europe/US, a high incidence of renal calculi (1.9%) has been noted, however, the causal relationship to zonisamide is disputed. Indeed, although urinary lithiasis has also been recorded for patients in Japan, the aetiology, incidence and spontaneous regression of this condition suggest that it is not a serious problem for this patient population. Until this difference is clarified, it is likely that zonisamide will find its greatest use in the treatment of patients in Japan. Like many other established antiepileptic drugs, available data suggest the propensity for zonisamide to alter the pharmacokinetic profile of other anticonvulsant agents, although severe interactions appear to be unlikely.
The ultimate positioning of zonisamide in the therapy of epilepsy awaits clearer definition of its pharmacokinetic, efficacy (particularly in comparison with other antiepileptics) and tolerability profiles. At present therefore, available data do not support the use of this drug in individuals outside of Japan, except in formal clinical studies involving careful monitoring. However, for patients in Japan with epilepsies refractory to established therapy, zonisamide would appear a valid alternative, particularly in the treatment of partial seizures.
Pharmacodynamic Properties
The antiepileptic effects of zonisamide have been demonstrated in animal models of epilepsy through study of electroencephalographic (EEG) activity and the symptoms of induced seizures. Indeed, assessment of EEG recordings of focal and secondarily generalised seizures evoked by a variety of stimuli in the cortex or subcortex of cats and/or rats administered zonisamide revealed attenuation or abolition of seizure activity and its spread. In most animal models, afterdischarges were shortened in duration and their thresholds elevated.
Zonisamide has also shown activity in animal studies which have concentrated on the symptoms of induced seizures. Thus, zonisamide consistently prevented the tonic extensor component of maximal electroshock seizures, attenuated or controlled fully kindled seizures and abolished the maximal seizures induced by pentylenetetrazole. In contrast, zonisamide neither had effect on the minimal seizures induced by pentylenetetrazole, nor on convulsive death induced by strychnine.
In the above studies zonisamide demonstrated an antiepileptic profile most similar to that of phenytoin or carbamazepine.
The pharmacodynamic profile of zonisamide in animal models of epilepsy suggests that the anticonvulsant action of this drug involves blockade of the spread or propagation of seizure discharges and suppression of the epileptogenic focus. While full details of its mode of action are unknown, inhibition of neuronal voltage-dependent sodium and/or T-type calcium channels has been suggested.
There appears to be a wide margin between doses of zonisamide that are effective in animal models of epilepsy and those that produce adverse effects in the central nervous system (CNS) of animals, both in terms of signs of CNS effects and changes in EEG activity. Moreover, compared with other antiepileptic drugs, zonisamide showed less of a propensity to induce CNS effects. In accordance with such findings, acute lethal toxicity of zonisamide occurred at doses greater than most standard antiepileptic drugs. With regard to motor function, zonisamide depressed the feline flexor reflex, but was without effect on neuromuscular transmission.
Pharmacokinetic or pharmacodynamic tolerance to the anticonvulsive effects of zonisamide in animal models does not appear to occur with repeated administration, or in the presence of drugs that inhibit or induce microsomal enzymes.
Pharmacokinetic Properties
The pharmacokinetic profile of zonisamide has been assessed in volunteers in Japan or the US. Peak plasma concentrations (Cmax) following oral zonisamide ranged from 2.3 mg/L after a 200mg dose to 12.5 mg/L after an 800mg dose and were achieved within 2.4 to 3.6 hours in healthy volunteers in the US; area under the plasma concentration-time curve (AUC) increased dose-proportionally. The presence of food does not affect the rate or extent of zonisamide absorption. Zonisamide was highly concentrated in erythrocytes, with concentrations exceeding those in plasma by 4- to 9-fold in healthy volunteers in Japan. The blood pharmacokinetic profile of zonisamide (400mg) in patients with refractory epilepsy receiving concurrent anticonvulsive medication in the US, showed similarities to that in healthy volunteers with evidence of erythrocyte accumulation.
In Japan, repeat administration of zonisamide at dosages of up to 13 mg/kg/day to children, and 18.6 mg/kg to adults, resulted in plasma concentrations linearly proportional to the dose given; however, when administered in a multiple dose regimen to patients in the US, zonisamide exhibited nonlinear pharmacokinetics. Indeed, at steady-state, the clearance of zonisamide 200 to 600mg twice daily was only 42% of that following administration of a single 400mg dose. In clinical studies, plasma zonisamide concentrations of 7 to 40 mg/L have been associated with antiepileptic effects in patients receiving concomitant anticonvulsant therapies, although most patients showed signs of toxicity with doses resulting in plasma levels of >30 mg/L. Based on these results, a target steady-state plasma zonisamide concentration of 20 mg/L has been suggested.
Although no human data are available regarding the volume of distribution (Vd) of zonisamide at steady-state, Vd values were reduced from 1.8 L/kg after a single 200mg dose to 1.2 L/kg after an 800mg dose in studies which recruited volunteers in the US, reflecting nonlinear binding to erythrocytes. For the purpose of therapeutic monitoring, it is recommended that zonisamide concentrations are determined in plasma or serum. Plasma protein binding of zonisamide is nonsaturable and is not extensive (<50%) over therapeutic plasma concentrations.
In studies which recruited volunteers in the US, the plasma clearance rate was 1.34 L/h at doses of 200 or 400mg, but clearance was reduced by 22% after a dose of 800mg. Plasma elimination half-life ranged from 50 to 68 hours after single oral doses of 200 to 800mg.
Urinalysis has revealed that zonisamide undergoes biotransformation by acetylation and also cleavage of the isoxazole ring followed by conjugation with glucuronic acid. In Japan, the parent drug and glucuronide conjugate have accounted for almost 50% of a 200mg dose recovered in the urine of volunteers. In animal studies, an appreciable portion of zonisamide has been recovered from faeces; however, whether this route is of importance in man awaits clarification. Available data suggest that disposition of single dose zonisamide is unaffected by the presence of renal dysfunction in volunteers in the US.
Clinical Efficacy
Most of the published clinical trials of zonisamide have been conducted in Japan. Supportive clinical trials conducted later in the US and Europe have generally not been published in full. This review has therefore focused on the efficacy of zonisamide in patients recruited to clinical studies in Japan.
The efficacy of zonisamide has been demonstrated in a total of 1008 adults or children with various epilepsies (mainly refractory to treatment), recruited to a series of predominantly non-comparative clinical trials in Japan. In this population, oral administration of zonisamide at mean dosages of 5.9 to 8.8 mg/kg/day resulted in mean serum concentrations of about 20 mg/L. Efficacy, defined as a reduction in seizure frequency of ⩾50% compared with baseline, varied with seizure type, seizure frequency and number of concomitant antiepileptic medications. In this analysis zonisamide was particularly beneficial in the treatment of partial seizures (partial-onset generalised tonic-clonic, simple and/or complex seizures) with efficacy rates (⩾50% reduction in seizure frequency compared with baseline) of 50 to 60%. Zonisamide was also effective, although to a more variable degree, in the treatment of generalised or compound/combination seizures. In large patient groups (n ⩾ 46) efficacy rates were 59% for those with generalised tonic-clonic seizures, 26% for those with generalised tonic seizures and 41% for those with compound/combination seizures. Other generalised seizures also responded to therapy with zonisamide although the patient population was relatively small (n ⩽ 10); notably zonisamide was effective in the treatment of West Syndrome and Lennox-Gastaut Syndrome. In the long term (⩾1 year), efficacy rates for zonisamide in 155 epileptic patients exceeded 60%, except in patients with generalised tonic (40%) or compound/combination seizures (50%). In comparative clinical trials conducted in Japan, the efficacy of zonisamide was judged equivalent to that of carbamazepine in patients with predominantly partial epilepsies, and valproic acid in limited numbers of paediatric patients (n = 32) with convulsive or nonconvulsive generalised seizures. In broad agreement with these findings, superior efficacy has been attributed to zonisamide when compared with placebo in a European study of patients with complex partial seizures. Furthermore, the efficacy of zonisamide in the treatment of partial seizures has also been documented in a noncomparative study conducted in the US.
Tolerability
In a series of principally noncomparative clinical trials which recruited 1008 adults or children with epilepsy in Japan, zonisamide was associated with an adverse event rate of 51% and a withdrawal rate of 18% in the presence of 0 to ⩾3 concomitant antiepileptic drugs. Principal adverse events were drowsiness (24% of patients), ataxia (13%), loss of appetite (11%), gastrointestinal problems (7%), loss of or decreased spontaneity (6%), and slowing of mental activity (5%). Increased serum transaminase enzyme activity or leucopenia necessitated the withdrawal of 2% of patients. Monotherapy/polytherapy (considered together) was associated with marginally greater incidences of adverse events (particularly drowsiness), than monotherapy alone. In a comparative clinical trial conducted in patients in Japan, the tolerability profile for zonisamide was comparable with that for carbamazepine, although ataxia was noted more frequently with carbamazepine and anorexia occurred more frequently with zonisamide.
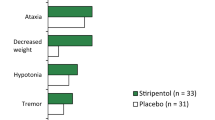
Most of the adverse events recorded in a placebo-controlled investigation conducted in Europe and a noncomparative investigation conducted in the US related to the nervous or gastrointestinal systems. However, renal calculi were noted for 4 of 113 patients (3.5%) in the latter study (2 with familial association), and for 13 of 700 patients (1.9%). recruited to nonconiparative studies conducted in the US/Europe. Nevertheless, a causal relationship to zonisamide is disputed. Indeed, differences in the incidence of urinary lithiasis appear to exist, since renal calculi were noted infrequently (0.2%) among 1008 patients in Japan and affected patients showed spontaneous regression of this condition with a familial predisposition.
Zonisamide adversely affected specific cognitive function such as acquisition and consolidation in patients in the US at plasma concentrations of >30 mg/L; however, other findings suggested tolerance to the adverse cognitive effects observed.
Dosage and Administration
Zonisamide is available in Japan in tablet (100mg) or powder form (200 mg/g) and may be orally administered once daily or in 2 or 3 divided doses. In Japan, the recommended initial adult dosage is 100 to 200 mg/day, increasing if necessary to 200 to 400 mg/day (maximum 600 mg/day). Children in Japan may be treated initially with dosages of 2 to 4 mg/kg/day, increasing to 4 to 8 mg/kg/day (maximum 12 mg/kg/day). Dosage adjustments may be made at 1- to 2-week intervals and optimum therapy may be achieved through monitoring of plasma/serum concentrations. No dosage recommendations are available for patients in countries other than Japan.
Zonisamide should not be abruptly discontinued and should be administered with caution to patients with hepatic dysfunction and pregnant women.
Blood zonisamide concentrations may alter with concomitant administration of other antiepileptic drugs. Indeed, blood AUC values for zonisamide were greater in the presence of carbamazepine than in the presence of phenytoin, and phenobarbital has been associated with increased zonisamide plasma clearance. Studies which have evaluated the effects of zonisamide on the disposition of other concomitant antiepileptic drugs have shown inconsistent findings. Together, these results suggest that severe interactions are unlikely to occur between zonisamide and other antiepileptic drugs although dosage adjustment may be necessary with polytherapy.
Similar content being viewed by others
References
Adams PR, Galvin M. Voltage-dependent current of vertebrate neurons and their role in membrane excitability. In Delgado-Escueta et al. (Eds.) Basic mechanisms of the epilepsies, advances in neurology, pp. 137–170, Vol. 44, Raven Press, New York, 1986
Annegers JF, Elveback LR, Hauser WA, Kurland LT. Do anticonvulsants have a teratogenic effect? Archives of Neurology 31: 364, 1974
Anon. Dainippon’s zonisamide anti-epileptic enters phase III clinicals. FDC Reports, T&G-5, 29 June 1992
Azzaro AJ, Wenger GR, Graig CR, Stitzel RE. Reserpine-induced alterations in brain amines and their relationship to changes in the incidence of minimal electroshock seizures in mice. Journal of Pharmacology and Experimental Therapeutics 180: 558–568, 1972
Barsa JA, Kline NS. Treatment of two hundred disturbed psychotics with reserpine. Journal of the American Medical Association 158: 110–113, 1955
Bartoszyk GD, Hamer M. The genetic animal model of reflex epilepsy in the Mongolian gerbil: differential efficacy of new anticonvulsive drugs and prototype antiepileptics. Pharmacological Research Communications 19: 429–441, 1987
Berent S, Sackellares C, Giordani B, Wagner JG, Dornofrio PD, et al. Zonisamide (CI-912) and cognition: results from preliminary study. Epilepsia 28: 61–67, 1987
Berry DJ. Determination of zonisamide (3-sulphamoylmethyl-1,2-benzisoxazole) in plasma at therapeutic concentrations by high performance liquid chromatography. Journal of Chromatography 534: 173–181, 1990
Bowman WC, Rand MJ. Textbook of pharmacology, p. 14.16. Blackwell Scientific Publications, Oxford, 1980
Browne TR, Szabo GK, Kres J, Pylilo RJ. Drug interactions of zonisamide (CI-912) with phenytoin and carbamazepine. Abstract. Journal of Clinical Pharmacology 26: 555, 1986
Chen G, Ensor C, Bohner B. A facilitation action of reserpine on the central nervous system. Proceedings of the Society for Experimental Biology and Medicine 86: 507–510, 1954
Commission on Antiepileptic Drugs of the International League Against Epilepsy. Proposal for revised clinical and electroencephalographic classification of epileptic seizures. Epilepsia 22: 489–501, 1989
Cornford EM, Landon KP. Blood-brain barrier transport of CI-912: single passage equilibration of erythrocyte-borne drug. Therapeutic Drug Monitoring 7: 247–254, 1985
Eadie MJ. Neurological diseases: seizure disorders. Speight (Ed.) Avery’s drug treatment, pp. 1089–1103, Adis Press Ltd, Auckland, New Zealand, 1987
Fromm GH, Shibuya T, Terrence CF. Effect of zonisamide (CI-912) on a synaptic system model. Epilepsia 28: 673–679, 1987
Fukushima Y, Kaneko S, Sato T. Study of zonisamide, a new antiepileptic drug in refractory epilepsy (in Japanese). Journal of Clinical Therapeutics and Medicine 2: 1179–1187, 1986
Graves NM, Leppik IE. Antiepileptic medications in development. DICP: Annals of Pharmacotherapy 25: 978–986, 1991
Hamada K, Ishida S, Yagi K, Seino M. Anticonvulsant effects of zonisamide on amygdaloid kindling in rats. Neurosciences 16: 407–412, 1990
Hammond EJ, Perchalski RJ, Wilder BJ, McLean JR. Neuropharmacology of zonisamide, a new antiepileptic drug. General Pharmacology 18: 303–307, 1987
Hasegawa S, Kaji S, Sasagawa M, Ito N, Matsui N, et al. A clinical evaluation of zonisamide (ZNS, AD-810) on partial epilepsy (in Japanese). Rinsho Iyaku 4: 2385–2395, 1988
Henry TR, Sackellares JC. Zonisamide. In Resor Jr et al. (Eds.) The medical treatment of epilepsy, pp. 423–427, Marcel Dekker Inc., New York, 1992
Higuchi T, Igarashi Y, Watanabe Y, Yamauchi T. Clinical experience of zonisamide (AD-810), a new antiepileptic drug for refractory epilepsy (in Japanese). Rinsho Iyaku 3: 711–720, 1987
Hori M, Ito T, Oka M, Noda Y, Matsuno Y, et al. General pharmacology of the novel antiepileptic compound zonisamide — 1st communication: effects on the central nervous system. Arzneimittel-Forschung/Drug Research 37: 1124–1130, 1987
Ibba M, Vanasia A, Testa R. Differential antagonism of denzinol to various components of metrazol-induced seizures in rats and mice. Pharmacological Research Communications 17: 1169–1180, 1985
Iinuma K, Handa I, Fueki N, Yamamoto K, Kojima A, et al. Effects of zonisamide (AD-810) on refractory epilepsy in children: special reference to temporal lobe abnormalities. Current Therapeutic Research 4.3: 281–290, 1988
Ikoma R, Shimizu A. Long term efficacy and safety of zonisamide in treatment of epilepsy (in Japanese). Rinsho Iyaku 6: 185–193, 1990
Ito T, Hori M, Kadokawa T. Effects of zonisamide (AD-810) on tungstic acid gel-induced thalamic generalised seizures and conjugated estrogen-induced cortical spike-wave discharges in cats. Epilepsia 27: 367–374, 1986
Ito T, Hori M, Masuda Y, Yoshida K, Shimizu M. 3-Sulfamoylmethyl-1,2-benzisoxazole, a new type of anticonvulsant drug; electroencephalographic profile. Arzneimittel-Forschung/Drug Research 30: 603–609, 1980
Ito T, Yamaguchi T, Miyizaki H, Sekine. Y, Shimizu M, et al. Pharmacokinetic studies of AD-810, a new antiepileptic compound. Arzneimittel-Forschung/Drug Research 32: 1581–1586, 1982
Juergens U. HPLC analysis of antiepileptic drugs in blood samples: microbore separation of fourteen compounds. Journal of Liquid Chromatography 10: 507–532, 1987a
Juergens U. Simultaneous determination of zonisamide and nine other antiepileptic drugs and metabolites in serum. A comparison of microbore and conventional high-performance liquid chromatography. Journal of Chromatography 385: 233–240, 1987b
Kaibe K, Nishimura S, Ishii H, Sunahara N, Naruto S, et al. Competitive binding enzyme immunoassay for zonisamide, a new antiepileptic drug, with selected paired-enzyme labelled antigen and antibody. Clinical Chemistry 36: 24–27, 1990
Kagono Y, Suitsu N, Murata A, Kinoshita T, Saitoh S, et al. Treatment of epilepsy with zonisamide (ZNA), a new antiepileptic drug (in Japanese). Igaku to Yakugaku 18 (Suppl.): 1641–1649, 1987
Kakegawa N. An experimental study on the modes of appearance and disappearance of suppressive effect of antiepileptic drugs on kindled seizure. Psychiatria et Neurologia Japonica 88: 81–98, 1986
Kamei C, Oka M, Masuda Y, Yoshida K, Shimizu M. Effects of 3-sulfamoylmethyl-1,2-benzisoxazole (AD-810) and some antiepileptics on the kindled seizures in the neocortex, hippocampus and amygdala in rats. Archives Internationales de Pharmacodynamie et de Therapie 249, 164–176, 1981
Kanazawa O, Sengoku A, Kawai I. A clinical trial of zonisamide (ZNA), a new antiepileptic drug on adults and children with refractory epilepsy (in Japanese). Rinsho Iyaku 3 (Suppl.): 1181–1186, 1987
Kimura M, Tanaka N, Kimura Y, Miyake K, Kitaura T, et al. Factors influencing serum concentration of zonisamide in epileptic patients. Chenfical and Pharmaceutical Bulletin 40: 193–195, 1992
Kohsaka M, Sumi T, Chiba T, Tanaka S, Mori N, et al. The long term treatment of zonisamide for epileptic patients with intractable epilepsy (in Japanese). Rinsho Iyaku 3: 1343–1352, 1987
Kumagai N, Seki T, Yamawaki H, Suzuki N, Kimiya S, et al. Monotherapy for childhood epilepsies with zonisamide. Japanese Journal of Psychiatry and Neurology 45: 357–359, 1991
Leppik IE, Gumnit RJ, Jacobs MP. Zonisamide in myoclonic epilepsy: a case report. Epilepsia 26: 537, 1985
Leppik IE, Gumnit RJ, Jacobs MP, Henry T. Intractable myoclonic seizures treated with zonisamide. Neurology 36 (Suppl.): 326, 1986
Leppik IE, Willmore LJ, Homan RW, Fromm G, Dommen KJ, et al. Efficacy and safety of zonisamide: results of a multicenter study. Epilepsy Research 14: 165–173, 1993
Lerman P. Seizures induced or aggravated by anticonvulsants. Epilepsia 28: 706–710, 1986
Liao W, Nishimura S, Yagi K, Seino M. Determination of serum zonisamide concentration by the use of enzyme immunoassay technique. Journal of Clinical Laboratory Instrumentation and Reagents 12: 429–432, 1989
Loiseau P, Schmidt D, Deisenhammer E, Despland PA, Egli M, et al. Efficacy of zonisamide in the treatment of complex partial seizures in medically refractory patients. Abstract. Proceedings of the 17th Epilepsy International Congress, p73, 1987
Masuda Y, Karasawa T, Shiraishi Y, Hori M, Yoshida K, et al. 3-Sulphamoylmethyl-1,2-benzisoxazole, a new type of anticonvulsant drug. Pharmacological profile. Arzneimittel-Forschung/Drug Research 30: 477–483, 1980
Masuda Y, Utsui Y, Shiraishi Y, Karasawa T, Yoshida K, et al. Pharmacokinetic and pharmacodynamic tolerance of a new anticonvulsant agent (3-sulphamoylmethyl-1,2-benzisoxazole) compared to phenobarbitone, diphenylhydantoin and carbamazepine in rats. Archives Internationales de Pharmacodynamie et de Therapie 240: 79–89, 1979
Matsumoto K, Miyazaki H, Fujii T, Amejima H, Furukawa H, et al. Binding of sulfonamides to erythrocyte proteins and possible drug-drug interaction. Chemical and Pharmaceutical Bulletin 37: 2807–2810, 1989a
Matsumoto K, Miyazaki H, Fujii T, Hashimoto M. Binding of sulfonamides to erythrocytes and their components. Chemical and Pharmaceutical Bulletin 37: 1913–1915, 1989b
Matsumoto K, Miyazaki H, Fujji T, Kagemoto A, Maeda T, et al. Absorption, distribution and excretion of 3-(sulphamoyl[14C]methyl)-1,2-benzisoxazole (AD-810) in rats, dogs and monkeys and of AD-810 in men. Arzneimittel-Forschung/Drug Research 33: 961–968, 1983
McLean MJ, Macdonald RL. Multiple actions of phenytoin on mouse spinal cord neurones in cell culture. Journal of Pharmacology and Experimental Therapeutics 227: 779–789, 1983
Millichap JG. Relation of laboratory evaluation to clinical effectiveness of antiepileptic drugs. Epilepsia 10: 315–328, 1969
Mimaki T, Suzuki Y, Tagawa T, Tanaka J, Itoh N, et al. [3H]Zonisamide binding in rat brain. Japanese Journal of Psychiatry and Neurology 42: 640–642, 1988a
Mimaki T, Tagawa T, Shudo N, Sugimoto T, Matsuoka S, et al. Therapeutic efficacy and blood concentrations of zonisamide (AD-810) in epileptic children (in Japanese). Rinsho Yakuri 19: 143–144, 1988b
Murasaki M, Inami M, Takahashi A, Otani Y, Yamazumi S, et al. A clinical phase II study of a new antiepileptic, zonisamide (AD-810) in refractory seizures (in Japanese). Rinsho Iyaku 3: 693–709, 1987
Naito H, Itoh N, Matsui N, Eguchi T. Monitoring plasma concentrations of zonisamide and clonazepam in an epileptic attempting suicide by an overdose of the drugs. Current Therapeutic Research 43: 463–467, 1988
Nakatsuji K, Matsuno Y, Nakamura N, Fujitani B, Ito T, et al. General pharmacology of the novel antiepileptic compound zonisamide — 2nd communication: effects on cardiovascular, visceral, renal and blood functions. Arzneimittel-Forschung/Drug Research 37: 1131–1136, 1987
Nishiguchi K, Ohnishi N, Iwakawa S, Yagi J, Nakayama S-I, et al. Pharmacokinetics of zonisamide: sataurable distribution into human and rat erythrocytes and into rat brain. Journal of Pharmacobio-Dynamics 15: 409–415, 1992
Nishiura N, Oiwa T. Use of a new antiepileptic drug, AD-810 (zonisamide, ZNS) — long term treatment of intractable epilepsy patients (in Japanese). Yakuri To Shinryo 15 (Suppl.): 4215–4223, 1987
Noguchi H, Tomita N, Yoshida K, Maeda T, Arakawa S, et al. Simultaneous HPLC determination of zonisamide and other antiepileptic drugs in human serum (in Japanese). Yakuri to Chiryo 16: 4805–4811, 1988
Ogata A, Numata Y, Miyamoto K, Miyakawa T. Treatment of epilepsy with a new antiepileptic drug zonisamide (phase III study) — single agent therapy and multiple drug therapy (in Japanese). Seishinka Chiryogaku 2 (Suppl.): 433–439, 1987
Oguni H, Hayakawa T, Fukuyama Y. Treatment of refractory paediatric epilepsy with zonisamide (AD-810) [in Japanese]. Tenkan Kenkyu 7 (Suppl.): 43–50, 1989
Oguni H, Hayashi K, Fukuyama Y, Iinuma K, Seki T, et al. Phase III study of AD-810 [zonisamide (ZNS)], a new antiepileptic, in the treatment of paediatric epilepsy (in Japanese). Shonika Rinsho 41 (Suppl.): 439–450, 1988
Ojemann LM, Shastri RA, Wilensky AJ, Friel PN, Levy R, et al. Comparative pharmacokinetics of zonisamide (CI-912) in epileptic patients on carbamazepine or phenytoin monotherapy. Therapeutic Drug Monitoring 8: 293–296, 1986
Okuno T. Clinical experience of zonisamide (ZNS), treatment of paediatric epilepsy (in Japanese). Rinsho to Kenkyu 68: 841–842, 1991
Ono T, Takahashi Y, Kan R, Sonobe N, Amamura I, et al. Clinical experience of zonisamide (AD-810) on refractory epilepsy (in Japanese). Journal of Clinical Therapeutics and Medicines 2: 1313–1320, 1986
Ono T, Yagi K, Seino M. Clinical efficacy and safety of a new antiepileptic drug, zonisamide — a multi-institutional phase III study (in Japanese). Seishin Iyaku 30: 471–482, 1988
Ota Y, Nakane Y, Hironaka I, Takahashi K, Miyahara A, et al. Therapeutic effect of zonisamide (AQ-810, ZNS), on refractory epilepsy (in Japanese). Rinsho Iyaku 3 (Suppl.): 1079–1087, 1987
Reynolds EH, Shorvon SD. Single drug or combination therapy for epilepsy. Drugs 21: 374–382, 1981
Reynolds EH, Travers RD. Serum anticonvulsant concentrations in epileptic patients with mental symptoms — a preliminary report. British Journal of Psychiatry 124: 440–445, 1974
Rock DM, McDonald RL, Taylor CP. Blockade of sustained repetitive action potentials in cultured spinal cord neurons by zonisamide (AD-810, CI 912), a novel anticonvulsant. Epilepsy Research 3: 138–143, 1989
Sackellares JC, Donofrio PD, Wagner JG, Abou-Khalil B, Berent S, et al. Pilot study of zonisamide (1,2-Benzisoxazole-3-methanesulphonamide) in patients with refractory partial seizures. Epilepsia 26: 206–211, 1985
Sakamoto T, Nakazawa Y, Kotorii T, Nakamura J, Nonaka K, et al. Clinical experience with zonisamide (AD-810, ZNA), a new antiepileptic in refractory seizures (in Japanese). Rinsho to Kenkyu 64: 4014–4024, 1987
Schauf CL. Zonisamide enhances slow sodium inactivation in Myxicola. Brain Research 413: 185–188, 1987
Schentag JJ, Gengo FM, Wilton JH, Sedman AJ, Grasela TH, et al. Influence of phenobarbital, cimetidine, and renal disease on zonisamide kinetics. Abstract. Pharmaceutical Research 4 (Suppl.): S–79, 1987
Seino M, Miyazaki H, Ito T. Zonisamide. In Pisani et al. (Eds) New antiepileptic drugs (Epilepsy Research Suppl. 3), pp. 169–174, Elsevier Science Publishers, Amsterdam, 1991
Seino M, Ohkuma T, Miyasaka M, Manaka S, Takahashi R, et al. Efficacy evaluation of AD-810 (zonisamide) — results of a double-blind comparison with carbamazepine (CBZ) [in Japanese]. Igaku no Ayumi 144: 275–291, 1988
Shields WD, Saslow E. Myoclonic, atonic and absence seizures following institution of carbamazepine therapy in children. Neurology 33: 1487–1489, 1983
Shimizu A, Ikoma R, Shimizu T. Effects and side effects of zonisamide during long term medication. Current Therapeutic Research 47: 696–706, 1990
Shimizu A, Yamamoto J, Yamada Y, Tanaka M, Kawasaki T. The antiepileptic effect of zonisamide in patients with refractory seizures. Current Therapeutic Research 42: 147–155, 1987
Shimizu A, Yamamoto J, Yamada Y, Tanaka M, Kawasaki T. The antiepileptic effect of zonisamide on patients with refractory seizures and its side effect. Japanese Journal of Psychiatry and Neurology 42: 583, 1988
Shorvon SD. Epidemiology, classification, natural history and genetics of epilepsy. Lancet 336: 93–96, 1990
Shuto H, Sugimoto T, Yasuhara A, Hatanaka T, Woo M, et al. Efficacy of zonisamide in children with refractory partial seizures. Current Therapeutic Research 45: 1031–1036, 1989
Siedlik P, Brockbrader H, Chang T, Latts J, Sedman A. Effect of food on the oral absorption of zonisamide in normal healthy volunteers. Pharmaceutical Research 3 (Suppl.), 158S, 1986
Snead OC, Hosey LC. Exacerbation of seizures in children by carbamazepine. New England Journal of Medicine 313: 916–921, 1985
Suzuki S, Kawakami K, Nishimura S, Watanabe Y, Yagi K, et al. Zonisamide blocks T-type calcium channel in cultured neurons of rat cerebral cortex. Epilepsy Research 12: 21–27, 1992
Suzuki N, Seki T, Yamawaki H, Yamada T, Kumagaya N. Treatment of paediatric epilepsy with AD-810 (zonisamide — ZNS) [in Japanese]. Japanese Journal of Paediatrics 40 (Suppl.): 3147–3152, 1987
Swinyard EA. In Mercer (Ed.) Anticonvulsant drugs, pp. 47–65, Pergamon Press, New York, 1973
Tagawa T, Mimaki T, Shuto H, Sugimoto T, Matsuoka O, et al. Treatment of paediatric epilepsy with AD-810 (zonisamide-ZNS) — efficacy of treatment and blood levels (in Japanese). Shonika Shinryo 51 (Suppl.): 539–543, 1988
Takahashi I, Nomura K, Yamamoto N, Furune S. Efficacy of zonisamide for intractable epilepsy in childhood. Brain and Development 9: 136, 1987
Takeda A, Inaguma J, Shimizu S. Treatment of intractable epilepsy with a new antiepileptic drug, zonisamide (AD-810), with special reference to dosage reduction of concurrent drugs (in Japanese). Japanese Pharmacology and Therapeutics 15: 4225–4233, 1987
Taylor CP, McLean JR, Brockbrader HN, Buchanan RA, Karasawa T, et al. Zonisamide (AD-810, CI-912). In Meldrum & Porter (Eds) New anticonvulsant drugs, pp. 277–294, John Libbey, London, 1986
Twombly DA, Narahashi T. Phenytoin block of low threshold calcium channels is voltage- and frequency dependent. Abstract. Society for Neuroscience 12: 1193, 1986
Uesugi H, Miyasaka M, Matsuura M, Ohtaka T, Takahashi R. Zonisamide (AD-810, ZNS) in epilepsy therapy (in Japanese). Rinsho Seishin Igaku 15 (Suppl.): 2021–2028, 1986
Uno H, Kurokawa M, Masuda Y, Nishimura H. Studies on 3-substituted 1,2 benzisoxazole derivatives. Syntheses of 3-(sufamoylmethyl)-1,2-benzisoxazole derivatives and their anticonvulsant activities. Journal of Medicinal Chemistry 22: 180–183, 1979
Uno H, Kurokawa M, Masuda Y. Syntheses of 2-sulfamoylmethylbenzoxazole derivatives and determination of their anticonvulsant activities. Chemical and Pharmaceutical Bulletin 29: 2359–2361, 1981
Wada Y, Hasegawa H, Okuda H, Yamaguchi N. Anticonvulsant activity of zonisamide and phenytoin on seizure activity of the feline visual cortex. Brain and Development 12: 206–210, 1990a
Wada Y, Hasegawa H, Yamaguchi N. Effect of a novel anticonvulsant, zonisamide (AD-810, CI-912), in an experimental model of photosensitive epilepsy. Epilepsy Research 7: 117–120, 1990b
Wagner JG, Sackellares JC, Donofrio PD, Berent S, Sakmar E. Nonlinear pharmacokinetics of CI-912 in adult epileptic patients. Therapeutic Drug Monitoring 6: 277–283, 1984
Wilensky AJ, Friel PN, Ojemann LM, Dodrill CB, McKormaick KB, et al. Zonisamide in epilepsy: a pilot study. Epilepsia 26: 212–220, 1985
Woodbury DM, Fingl E. In Goodman et al. (Eds) The pharmacological basis of therapeutics, pp. 201–206, McMillan Publishing Co., New York, 1975
Yagi K, Seino M. Methodological requirements for clinical trials in refractory epilepsies — our experience with zonisamide. Progress in Neuro-Psychopharmacology and Biological-Psychiatry 16: 79–85, 1992
Yagi K, Seino M, Mihara T, Tottori T, Numata Y, et al. Open clinical trial of a new antiepileptic drug, zonisamide (ZNA) on 49 patients with refractory epileptic seizures (in Japanese). Seishin Igaku 29: 111–119, 1987
Yamatogi Y, Ohtahara S. Proceedings of the International Symposium ‘New Trends in Paediatric Epileptology’, Okayama, Japan, 1990
Author information
Authors and Affiliations
Additional information
Various sections of the manuscript reviewed by: S. Berent, Department of Neurology and Psychiatry, College of Pharmacy, University of Michigan Medical Center, Ann Arbor, Michigan, USA; D.W. Chadwick, The University of Liverpool, Mersey Regional Department of Medical and Surgical Neurology, Walton Hospital, Liverpool, England; E.M. Cornford, Neuropharmacology Laboratories, West Los Angeles Veterans Administration Center, Los Angeles, California, USA; M. Dam, University Clinic of Neurology, Hvidovre Hospital, Hvidovre, Copenhagen, Denmark; M.J. Eadie, Department of Medicine, Clinical Science Building, Royal Brisbane Hospital, Brisbane, Queensland, Australia; G.H. Fromm, Department of Neurology, University of Pittsburgh School of Medicine, Pittsburgh, Pennsylvania, USA; M. Kimura, Department of Pharmaceutical Services, Hiroshima University Hospital, Hiroshima, Japan; H. Meinardi, Institut voor epilepsiebestrijding, Heemstede, The Netherlands; H. Oguni, Department of Paediatrics, Tokyo Women’s Medical College, Tokyo, Japan; L.M. Ojemann, Epilepsy Center, Harborview Medical Center, Seattle, Washington, USA; F. Pisani, Clinica Neurologica 1, Policlinico Universitario, Contesse-Messina, Italy; J.C. Sackellares, Department of Neurology, University of Michigan Medical Center, Ann Arbor, Michigan, USA; M. Seino, National Epilepsy Center, Shizuoka Higashi Hospital, Shizuoka, Japan; Y. Wada, Department of Neuropsychiatry, Kanazawa University School of Medicine, Kanazawa, Japan.
Rights and permissions
About this article
Cite this article
Peters, D.H., Sorkin, E.M. Zonisamide. Drugs 45, 760–787 (1993). https://doi.org/10.2165/00003495-199345050-00010
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199345050-00010