Summary
Pregnancy is a specific dynamic state, and the potential usefulness of caring for a disorder in the fetus or the mother is now well established. Previously, pregnant women have been excluded from clinical trials, therefore only a few studies concerning evaluation of the pregestational metabolism or transplacental transfer (TPT) of drugs exist.
Questions regarding the TPT of drugs are extensive and complex. For example, does TPT occur at a given gestational age, in the context of a particular type of pathology or when a drug is administered by a certain dosage regimen? If this is the case, what is the rapidity of penetration of the products of conception by the drug (bearing in mind its physicochemical characteristics)? Need harmful adverse effects on the child be feared? Is such penetration desirable, of no consequence, or dangerous? Does the possibility exist of accumulation in the placenta, fetal tissue or amniotic fluid? Should such findings modify the therapeutic regimens of drugs given to expectant mothers?
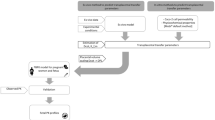
Exchange mechanisms are complicated and models developed in vitro only partially reflect the actual equilibria that exist between mother and fetus. These include: (i) the perfused cotyledon model, which while simple, elegant and inexpensive, offers only a localised, restricted and fixed view of pregnancy; (ii) isolated anatomical fractions that are informative, but which straddle the border between physiology and pharmacology; and (iii) the necessary study, using microsomes, of placental metabolic capacity (enzyme cartography). In vivo study of TPT is based upon various multicompartmental pharmacokinetic models, some of which have been relatively validated in animals. The simplest indicator for the in vivo evaluation of TPT of a drug in the human species is determination of a feto-maternal blood concentration ratio (usually performed at the time of placental separation). However, the usefulness and limitations of this parameter are controversial, and it would seem preferable to associate it with a pharmacokinetic profile of variations in blood concentrations established in the mother. Furthermore, any extrapolation of a single result to fetal and adjacent tissues must be done with the greatest caution.
Although, no drug should be used in pregnancy unless there is a clear therapeutic indication, study of the TPT of therapeutically useful agents is essential to the understanding of their metabolism and is a prerequisite to the safe use of medications during pregnancy.
Similar content being viewed by others
References
Stern L. Drug therapy in the perinatal period. In: Stern L, editor. Basic and therapeutic aspects of perinatal pharmacology. New York: Raven Press, 1980: 7–12
Yaffe SJ, Stern L. Clinical implications of perinatal pharmacology. In: Mirkin C, editor. Perinatal pharmacology therapeutics. New York: Academic Press, 1976: 355–428
Stern L. Placental transfer of drugs. In: Stern L, editor. Drug use in pregnancy. Sydney: Adis Health Science Press, 1984: 45–67
Krauer B, Krauer F, Hytten F. Drug prescribing in pregnancy. Edinburgh: Churchill Livingston, 1984
Bourget P, Fernandez H, Delouis C, et al. Pharmacokinetics of tobramycin in pregnant women: safety and efficacy of a once-daily dose regimen. J Clin Pharm Ther 1991; 16: 167–76
Reece EA, Hobbins JC, Mahoney MJ, et al. Medicine of the fetus and mother. Reece EA, editor. Philadelphia: Lippincott Company, 1994
Fox H, Agrafojo-Blanco A. Scanning electron microscopy of the human placenta in normal and abnormal pregnancies. Eur J Obstet Gynecol Reprod Biol 1974; 412: 45–50
Reynolds F, Knott C. Pharmacokinetics in pregnancy and placental drug transfer. Oxf Rev Reprod Biol 1990; 11: 389–449
Schaaps JP, Hustin J, Thoumsin HJ, et al. Physiologie placentaire. Encyclopedie médicochirurgicale (Paris) obstétrique 5005 A10, 1989; 10: 1–24
Forestier F, Sole Y, Aiach M, et al. Absence of transplacental passage of Fragmin (KABI) during the second and the third trimesters of pregnancy. Thromb Haemost 1992; 67: 180–1
Page EW. Transfer of materials across the human placenta. Am J Obstet Gynecol 1957; 74: 705–18
Seller MJ. Some aspects of placental function. Postgrad Med J 1965; 41: 189–93
Labaune JP. Pharmacocinétique; principes fondamentaux. Paris: Masson, 1988
Contractor SF. Metabolic and enzymatic activity of human trophoblast. In: Loke YW, Whyte A, editors. Biology of trophoblast. Oxford: Elsevier, 1983: 235–81
Bohn H, Dati F, Luben G. Human trophoblast specific products other than hormones. In: Loke YW, Whyte A, editors. Biology of trophoblast. Oxford: Elsevier, 1983: 317–52
Panigel M, Pascaud M, Brun JL. Une nouvelle technique de perfusion de l’espace intervilleux dans le placenta humain isolé. Pathol Biol 1967; 15: 821
Schneider H, Panigel M, Dancis J. Transfer across the perfused human placenta of antipyrine, sodium and leucine. Am J Obstet Gynecol 1972; 114: 822–8
Schneider H, Proegler M, Duft R. Transfer of antipyrine, H2O, L-glucose and aminobutyric acid across the in vitro perfused human placental lobe. In: Kaufmann P, Miller RK, editors. Trophoblast research. New York: Plenum Medical Book Co, 1987: 525–33
Earle WR. Production of malignancy in vitro: IV the mouse fibroblast, cultures and changes seen in the living cells. J Natl Cancer Inst 1943; 4: 165–212
Challier JC, Millo-Guerre M, Nandakumaran M, et al. Flow dependent transfer of antipyrine in the human in vitro. Reprod NutrDev 1983; 23: 41–50
Ghabrial H, Czuba MA, Stead CK. Transfer of acipimox across the isolated perfused human placenta. Placenta 1991; 12: 653–61
Henderson GI, Zhi-Qiang Hu, Johnson RF, et al. Acyclovir transport by the human placenta. J Lab Clin Med 1992; 120: 885–92
Schenker S, Dicke JM, Johnson RF, et al. Effect of ethanol on human placental transport of model amino acids and glucose. Alcohol Clin Exper Res 1989; 13: 112–9
Schneider H, Mohlen KH, Dancis J. Transfer of amino-acids across the in vitro perfused human placenta. Pediatr Res 1979; 13: 236–40
Krishna BR, King RG, Gu W, et al. Effect of indomethacin on materno-fetal amino acid transfer in the dual perfused human placental cotyledon. Reprod Fertil Dev 1990; 2: 597–602
Krishna BR, King RG, Brennecke SP. Acetylcholine output and materno-fetal alpha aminoisobutyric acid transfer in the perfused human placental lobule. Reprod Fertil Dev 1991; 3: 459–65
Akbaraly JP, Guibert S, Leng JJ, et al. Etude du passage transplacentaire de cinq antibiotiques par perfusion in vitro du placenta humain. Pathol Biol 1985; 33: 368–72
Gude NH, Rice GE, King RG, et al. Analysis of the responses of the fetal vessels of human perfused human placental lobule to acute infusions of arachidonic acid. Reprod Fertil Dev 1990; 2: 591–6
Kraczkowski J, Grudzien M, Zrubeck H, et al. Influence of betamethasone on the vascular resistance in human placenta perfusion in vitro. Ginekol Pol 1989; 60: 160–5
Karl PI, Fisher SE. Biotin transport in microvillous membrane vesicles, cultured trophoblasts, and isolated perfused human placenta. Am J Physiol 1992; 262: 302–8
Wier PJ, Miller RK, Maulik D, et al. Toxicity of cadmium in the perfused human placenta. Toxicol Appl Pharmacol 1990; 105: 156–71
Boadi WY, Yannai S, Urbach J, et al. Transfer and accumulation of cadmium and the level of metallothionein in perfused human placenta. Arch Toxicol 1991; 65: 318–23
Stulc J, Stulcova B, Smid M, et al. Parallel mechanisms of Ca++ transfer across the perfused human placental cotyledon. Am J Obstet Gynecol 1994; 170: 162–7
Leng JJ, Mbanzulu PN, Akbaraly JP, et al. Etude in vitro du passage transplacentaire du sulfate de chloroquine. Pathol Biol 1987; 35: 1051–4
Levitz M, Jansen V, Dancis J. Transfer and metabolism of cortico-steroids in perfused human placenta. Am J Obstet Gynecol 1978; 132: 363–6
Nandakumaran M, Eldeen AS. Transfer of cyclosporin in the perfused human placenta. Dev Pharmacol Ther 1990; 15: 101–5
Dancis J, Lee JD, Mendoza S, et al. Transfer and metabolism of dideoxynosine by the perfused human placenta. J Acquir Immune Defic Syndr 1993; 6: 2–6
Derewlany LO, Leeder JS, Kumar R, et al. The transport of digoxin across the perfused human placental lobule. J Pharmacol Exper Ther 1990; 256: 1107–11
Dancis J, Jansen V, Kayden HJ, et al. Transfer across perfused human placenta II: free fatty acids. Pediatr Res 1973; 7: 192–7
Elliot BD, Langer O, Schenker S, et al. Insignificant transfer of glyburide occurs across the human placenta. Am J Obstet Gynecol 1991; 165: 807–12
Challier JC, Nandakumaran M, Mondow F. Placental transport of hexoses: a comparative study with antipyrine and amino acids. Placenta 1985; 6: 497–504
Fisher SE, Karl PI. Histidine transfer across the human placenta characteristics in the isolated perfused human placenta and the effect of ethanol. Placenta 1990; 2: 157–65
Groom TM, Gautieri RF. Influence of a stable prostacyclin analogue (iloprost) and cyclooxygenase inhibition on angiotensin-II in the perfused human placenta. Res Commun Chem Pathol Pharmacol 1989; 66(1): 21–32
Dumas JC, Giroux M, Teixera MG. Etude du passage transplacentaire de l’interféron alpha 2a sur le modèle du cotylédon isolé perfusé. Therapie 1993; 48: 73–5
Dancis J. The transfer of nutrients across the perfused human placenta. Adv Nutr Res 1990; 8: 1–10
Gude NM, Krishna BR, King RG, et al. Effects of opioids on acetylcholine output of perfused human placental cotyledon. Placenta 1989; 10: 445–52
Boura AL, Brennecke SP, Gude NM, et al. Effects of opioids on acetylcholine release into fetal vessels of human perfused placental cotyledon. Prog Clin Biol Res 1990; 328: 359–62
Fortunato SJ, Bawdon RE. Determination of pentamidine transfer in the in vitro perfused human cotyledon with high performance liquid chromatography. Am J Obstet Gynecol 1989; 60: 759–61
Challier JC, Guerre-Millo M, Richard MO, et al. Transfert et échange d’antipyrine dans le lobule placentaire humain perfusé in vitro. Ann Biol Animale Biochim Biophys 1977; 17: 1107–15
Dickinson RG, Hooper WD, Wood B, et al. The effect of pregnancy in humans on the pharmacokinetics of stable isotope labelled phenytoin. Br J Clin Pharmacol 1989; 28: 17–27
Kluck RM, Cannell GR, Hooper WD, et al. Disposition of phenytoin and phenobarbitone in the isolated perfused placenta. Clin Exper Obstet Gynecol 1988; 15: 827–36
Kuhn DC, Walenga RW, Stuart MJ. Aprostacyclin analogue crosses the in vitro perfused human placenta and improves transfer in some pathologie states. Am J Perinatol 1991; 8: 179–84
Dancis J, Levitz M, Katz J. Transfer and metabolism of retinol by the perfused human placenta. NY Pediatr Res 1992; 32: 195–9
Urbach J, Mor L, Fuchs S, et al. Transplacental transfer of ritodrine and its effect on placental glucose and oxygen consumption in an vitro human placental cotyledon perfusion. Gynecol Obstet Invest 1991; 32: 10–4
Bawdon RE, Maberry MC, Fortunato SJ, et al. Trimethoprim and sulfamethoxazole transfer in the in vitro perfused human cotyledon. Gynecol Obstet Invest 1991; 31: 240–2
Karl PI, Fisher SE. Taurine transport by microvillous membrane vesicles and the perfused cotyledon of the human placenta. Am J Physiol 1990; 258: 443–51
Omarini D, Barzago MM, Aramayona J, et al. Theophylline transfer across human placental cotyledon during in vitro dual perfusion. J Med 1992; 23: 101–16
Fortunato SJ, Bawdon RE, Swan KF. Transfer of timentin (ticarcillin and clavulanic acid) across the in vitro perfused human placenta: comparison with other agents. Am J Obstet Gynecol 1992; 167: 1595–9
Fowler DW, Eadie MJ, Dickinson RG. Transplacental transfer and biotransformation studies of valproic acid and its glucuronide (s) in the perfused human placenta. J Pharmacol Exper Ther 1989; 249: 318–23
Soto P, Berrebi A, Grandjean H. In vitro placental transfer of AZT using the perfused human placental cotyledon model. 2nd Congress of European Society for Development Pharmacology; 1990; Italy: 1990; N42
Berrebi A, Dumas JC, Giroux M. AZT materno-fetal and fetomaternal transfer in an ex vivo study. VII International Conference on AIDS; 1991 June; Florence, Italy, WA 1048
Beer WH, Johnson RF, Guentzel MN, et al. Human placental transfer of zinc: normal characteristics and role of ethanol. Alcohol Clin Exper Res 1992; 16: 98–105
Page KR, Abramovich DR, Aggett PJ. The transfer of zinc across the term dually perfused human placental lobule. Q J Exper Physiol 1988; 73: 585–93
Essien FE, Afamefuma GC. Chloroquine and its metabolites in human cord blood, neonatal blood and urine after maternal medication. Clin Chem 1982; 28: 1148–52
Carter BL, Driscoll CE, Smith GD. Theophylline clearance during pregnancy. Obstet Gynecol 1986; 68: 555–9
Grella PV, di Lenardo L, Konishi de Toffoli G, et al. Antenatal theophylline: fetus and newborn. In: Cosmi EV, Di Renzo GC, editors. Proceedings of XI European Congress of Perinatal Medecine. Chur, Switzerland: Harwood Academic Publishers, 1989: 584–93
Dancis J, Jansen V, Kayden HJ, et al. Transfer across perfused human placenta III: effect of chain length on transfer of free fatty acids. Pediatr Res 1974; 8: 796–9
Dancis J, Jansen V, Levitz M. Transfer across perfused human placenta IV: effect of protein binding on free fatty acids. Pediatr Res 1986; 10: 5–10
Plaa GL. Cinétique de distribution des médicaments dans l’unité foeto-placentaire. Coll INSERM Pharmacologie Périnatale 1977; 73: 17–22
Nandakumaran M, Gardey CL, Challier JC, et al. Placental monoamine oxidase content and inhibition: effect of enzyme inhibition on maternofetal transfer of noradrenaline (norepinephrine) in the human placenta in vitro. Placenta 1983; 4: 57–64
Ostrea Jr EM, Porter T, Balun J, et al. Effect of chronic maternal drug addiction on placental drug metabolism. Dev Pharmacol Ther 1989; 12: 42–8
Lowry OH, Rosebrough NJ, Farr AL, et al. Protein measurement with the folin phenol reagent. J Biol Chem 1951; 193: 265–75
Omura T, Sato R. The carbon monoxide-binding pigment of liver microsomes. J Biol Chem 1964; 239: 2370–85
Van Petten GR, Hirsch GH, Cherrington AD. Drug-metabolising activity of the human placenta. Can J Biochem 1968; 46: 1057–61
Daubeze M, Cassand P, Migaud ML. Activation métabolique du benzo (a)pyrène par le liquide amniotique humain. C R Acad Sci 1986; 302: 625–8
Raghuram TC, Krishnaway K. Basic concepts of clinical pharmacokinetics. J Assoc Physicians India 1992; 40: 29–35
Szeto HH. Maternal-fetal pharmacokinetics and fetal doseresponse relationships. Ann NY Acad Sci 1989; 562: 42–55
Fernandez H, Bourget P, Delouis C. Fetal levels of tobramycin following maternal administration. Obstet Gynecol 1990; 76: 992
Minora T, Ventresca GP, Mariani I. Problemi di farmacocinetica in gravidanza rassegna bibliografica. Ann Ostet Ginecol Med Perinat 1990: 127; 159–73
Bourget P, Pons JC, Delouis C, et al. Flecainide distribution, transplacental passage and accumulation into the amniotic fluid during the third trimester of pregnancy. Ann Pharmacother 1994; 28: 1031–4
Szeto HH, Umans JG, Mc Farland J. A comparison of morphine and methadone disposition in the maternal-fetal unit. Am J Obstet Gynecol 1982; 143: 700–6
Luecke RH, Wosilait WD, Pearce BA, et al. A physiologically based computer model for human pregnancy. Teratology 1994; 49: 90–103
Golub MS, Eisele JH, Anderson JH. Maternal-fetal distribution of morphine and alfentanil in near-term sheep and rhesus monkeys. Dev Pharmacol Ther 1986; 9: 12–22
Michiels M, Hendriks R, Heykants J. On the pharmacokinetics of domperidone in animals and men. II: tissue distribution, placental and milk transfer of domperidone in the wistar rat. Eur J Drug Metab Pharmacokinet 1981; 6: 37–48
Laishley RS, Carson RJ, Reynolds F. Effect of adrenaline on placental transfer of bupivacaine in rabbits. Br J Anaesth 1988; 60: 330–1
Hamshaw-Thomas AH, Rogerson N, Reynolds F. Transfer of bupivacaine, lignocaine and pethidine across the rabbit placenta-influence of maternal protein binding and fetal flow. Placenta 1984; 5: 61–70
Vert P, Boutroy MJ, Morselli P. Placental transfer of drugs. In: Stern L, editor. Drug use in pregnancy. Sydney: Adis Health Science Press, 1984: 45–67
Pedersen H, Morishima HO, Finster M. Anaesthesia during pregnancy and parturition. In: Finster M, Eskes TKAB, editors. Drug therapy during pregnancy. London: Butterworths, 1985: 161–82
Moya F, Thorndike V. Passage of drug across the placenta. Am J Obstet Gynecol 1962; 84: 1778–98
Krauer B, Dayer P. Fetal drug metabolism and its possible clinical implications. Clin Pharmacokinet 1991; 21: 70–80
Morselli PL, Boutroy MJ, Bianchetti G, et al. Pharmacokinetics of antihypertensive drugs in the neonatal périod. Dev Pharmacol Ther 1989; 13: 190–8
Obata I, Yamato T, Hayashi S, et al. Pharmacokinetic study of aztreonam transfer from mother to fetus. Jpn J Antibiot 1990; 43: 70–80
Matsuda S, Oh K, Hirayama H, et al. Transplacental transfer and clinical application of aztreonam. Jpn J Antibiot 1990; 43: 700–5
Ito K, Hirose R, Tamaya T, et al. Pharmacokinetic and clinical studies on aztreonam in the perinatal period. Jpn J Antibiot 1990; 43: 719–26
Makinoda S, Negishi H, Ohkohchi T, et al. Basic and clinical studies on aztreonam in obstetric and gynecologic infections during the perinatal period. Jpn J Antibiot 1990; 43: 692–5
Yamamoto T, Yasuda J, Okada H, et al. Pharmacokinetic and clinical studies on aztreonam in the perinatal period in obstetric and gynecology. Jpn J Antibiot 1990; 43: 727–35
Sengoku K, Shimizu T, Haga H, et al. Pharmacokinetic and clinical studies on aztreonam in the perinatal period. Jpn J Antibiot 1990; 43: 686–91
Yerbi MS, Friel PN, Mac Cormick K, et al. Pharmacokinetics of anticonvulsants in pregnancy: alteration in plasma protein binding. Epilepsy Res 1990; 5: 223–8
Brown CEL, Christmas JT, Bawdon RE. Placental transfer of cefazolin and piperacillin in pregnancies remote from term complication by Rh isoimmunization. Am J Obstet Gynecol 1990; 163: 938–43
Cho N, Fukunaga K, Kunji K. Pharmacokinetic studies on cefsulodin in the perinatal period. Jpn J Antibiot 1989; 42: 2735–42
Bourget P, Fernandez H, Quinquis V, et al. Pharmacokinetics and protein binding of ceftriaxone during pregnancy. Antimicrob Agents Chemother 1993; 37: 54–9
Bourget P, Quinquis V, Fernandez H, et al. Pharmacocinétique clinique de la ceftriaxone au cours du troisième trimestre de la grossesse et étude de son passage transplacentaire dans deux cas. Pathol Biol 1993; 41: 242–8
Bourget P, Quinquis-Desmaris V, Fernandez H. Ceftriaxone distribution and protein binding between maternal blood and milk postpartum. Ann Pharmacother 1993; 27: 294–7
Amoura Z, Schermann JM, Wechsler B, et al. Transplacental passage of colchicine in familial Mediterranean fever [letter]. J Rheumatol 1994; 21: 383
Bourget P, Fernandez H, Bismuth H, et al. Transplacental passage of cyclosporin after liver transplantation. Transplantation 1990; 49: 663–4
Bourget P, Fernandez H, Delouis C. Accumulation of cyclosporin in the conceptus during the first trimester of pregnancy after liver transplantation. Transplantation 1991; 51: 1306–7
Bourget P, Fernandez H, Quinquis V, et al. Pharmacokinetics of cyclosporin A during pregnancy: monitoring of treatment and specific assays of cyclosporin, based on five liver transplant patients. J Pharm Biomed Anal 1993; 11: 43–8
Kanhai HH, Van-Kamp II, Moolenar AJ, et al. Transplacental passage of digoxin in severe rhesus immunization. J Perinat Med 1990; 18: 339–43
Hildebrandt R, Weitzel H, Warnke K, et al. Pharmacokinetics of fenoterol in pregnant and non-pregnant women. Eur J Clin Pharmacol 1993; 45: 275–7
Kofinas AD, Simon NV, Sagel H, et al. Treatment of fetal supraventricular tachycardia with flecainide acetate after digoxin failure. Am J Obstet Gynecol 1991; 165: 630–1
Yamamoto T, Yasuda J, Okada H, et al. Pharmacokinetic and clinical studies on flomoxef in the perinatal period in obstetrics and gynecology. Jpn J Antibiot 1991; 44: 686–96
Tamate K, Sengoku K, Ishikawa M, et al. Study on flomoxef in the perinatal period. Jpn J Antibiot 1991; 44: 643–51
Ito K, Mikamo H, Tamaya T, et al. Pharmacokinetic and clinical studies on flomoxef in perinatal period. Jpn J Antibiot 1991; 44: 683–8
Cho N, Fukunaga K, Kunii K, et al. Studies on flomoxef in the perinatal period. Jpn J Antibiot 1991; 44: 674–82
Matsuda S, Hirayama H, Oh K. Pharmacokinetic and clinical studies of flomoxef in perinatal period. Jpn J Antibiot 1991; 44: 669–73
Forestier F, Daffos F, Said R, et al. Passage transplacentaire du fluor. J Gynecol Obstet Biol Reprod 1990; 19: 171–5
Melkkila A, Kaila T, Kanto J, et al. Pharmacokinetics of glycopyrronium in parturients. Anesthesia 1990; 45: 634–7
Matzsch T, Bergquist D, Bergquist A, et al. No transplacental passage of standard heparin or an enzymatically depolymerized low molecular weight heparin blood. Coag Fibrinolysis 1991; 2: 273–8
Heikkila A, Renkonen O, Erkkola R. Pharmacokinetics and transplacental passage of imipenem during pregnancy. Antimicrob Agents Chemother 1992; 36: 2652–5
Menon RK, Cohen RM, Sperling MA, et al. Transplacental passage of insulin in pregnant women with insulin-dependant diabetes mellitus. N Engl J Med 1990; 323: 309–15
Goyer RA. Transplacental transport of lead. Environ Health Perspect 1990; 89: 101–5
Guay J, Gaudreault P, Boulanger A, et al. Lidocaine hydrocarbonate and lidocaine hydrochloride for cesarean section: transplacental passage and neonatal effects. Acta Anaesthesiol Scand 1992; 36: 722–7
Heikkila A, Pyykko K, Erkkola R, et al. The pharmacokinetic of mecillinam and pivmeccillinam in pregnant and nonpregnant. Br J Clin Pharmacol 1992; 33: 629–33
Hill NCW, Selinger M, Ferguson J, et al. The placental transfer of mifepristone (RU 486) during the second trimester and its influence upon maternal and fetal steroid concentration. Br J Obstet Gynecol 1990; 97: 406–11
Hill NW, Selinger M, Ferguson J, et al. Transplacental passage of mifepristone and its influence on maternal and fetal steroid concentration in the second trimester of pregnancy. Hum Reprod 1991; 6: 458–62
Gerdin E, Salmonson T, Lindberg B, et al. Maternal kinetics of morphine during labour. J Perinat Med 1990; 18: 479–87
Belfort MA, Saade GR, Moise Jr KJ, et al. Nimodipine in the management of preeclampsia: maternal and fetal effects. Am J Obstet Gynecol 1994; 171: 417–24
Boiko SS, Zherdev VP, Vikhliaeva EM, et al. The pharmacokinetics and pharmacodynamics of pentoxifylline (trental) in the third pregnancy trimester. Eksp Klin Farmakol 1992; 55: 52–5
Takeda A, Okada H, Tanaka H. Protein binding of four anti-epileptic drugs in maternal and umbilical cord serum. Epilepsy Res 1992; 13: 147–51
Kazzi NJ, Ilagan NB, Liang K, et al. Placental transfer of vitamin K1 in preterm pregnancy. Obstet Gynecol 1990; 75 (Pt 1): 334–7
Heikkila A, Erkkola R. Pharmacokinetics of piperacillin during pregnancy. J Antimicrob Chemother 1991; 28: 419–23
Bourget P, Fernandez H, Ribou F, et al. Faible passage transplacentaire de la prazosine (Alpress®) au cours du troisième trimestre de la grossesse. J Gynecol Obstet Biol Reprod (Paris) 1993; 22: 871–4
Doreangeon PH, Fay R, Marx-Chemla C, et al. Passage transplacentaire de l’association pyrimethamine-sulfadoxine lors du traitement anténatal de la toxoplasmose congénitale. Presse Med 1990; 19: 22–9
Fujimoto S, Akahane M, Tanaka T, et al. Pharmacokinetics and materno-fetal influence of ritodrine hydrochloride during the continuous treatment of threatened premature labor. Nippon Sanka Fujinka Gakkai Zasshi 1989; 41: 321–7
Bourget P, Fernandez H, Demirdjian S, et al. Détermination des rapports de concentrations sériques foeto-maternelles de la tobramycine à la naissance. Un modèle de pharmacocinétique réduite. Arch Fr Pediatr 1991; 48: 543–7
Johannessen SI. Pharmacokinetics of valproate in pregnancy: mother-fetus-newborn. Pharm Weekbl Sci 1992; 14: 114–7
Bourget P, Fernandez H, Delouis C, et al. Transplacental passage of vancomycin during the second trimester of pregnancy. Obstet Gynecol 1991; 78: 908–11
Schenker S, Johnson RF, King TS, et al. Azidothymidine (zidovudine) transport by the human placenta. Am J Med 1990; 299: 16–20
Gillet JY, Bongain A, Abrar D, et al. Etude préliminaire sur le passage transplacentaire de l’AZT (Rétrovir®). J Gynecol Obstet Biol Reprod 1990; 19: 177–80
Pons JC, Taburet AM, Singlas E, et al. Placental passage of azathiothymidine (AZT) during the second trimester of pregnancy: study by direct fetal blood sampling under ultrasound. Eur J Obstet Gynecol Reprod Biol 1991; 40: 229–31
Basso A, Fernandez A, Althabe O. Passage of mannitol from mother to amniotic fluid and fetus. Am J Obstet Gynecol 1977; 49: 628–31
Kivalo I, Saarikoski S. Placental transmission and fetal uptake of 14C dimethyltubocurarine. Br J Anaesth 1972; 44: 557–61
Kivalo I, Saarikoski S. Placental transfer of 14C dimethyltubocurarine during caesarian section. Br J Anaesth 1976; 48: 239–42
Sodha RJ, Schneider H. Sulphate conjugation of β2-adrenoreceptor stimulating drugs by platelet and placental phenol sulfotransferase. Br J Clin Pharmacol 1984; 17: 106–8
Juchau MR. The role of the placenta in developmental toxicology. In: Snell L, editor. Developmental toxicology. London, 1982: 189–209
Rane A, Von Bahr C, Orrenius S, et al. Drug metabolism in the human fetus. In: Boreus L, editor. Fetal pharmacology. New York: Raven Press, 1973: 287–303
Gabler WL, Hubbard GL. The metabolism of 5,5-diphenylhydantoin in non pregnant and rhesus monkeys. Arch Int Pharmacodyn Ther 1973; 203: 72–91
Rane A, Tomson G. Prenatal and neonatal drug metabolism in man. Eur J Clin Pharmacol 1980; 18: 9–15
Hamsham-Thomas A, Reynolds F. Placental transfer of bupivicaine, pethidine and lignocaine in the rabbit: effect of umbilical flow rate and protein content. Br J Obstet Gynaecol 1985; 92: 706–13
Knott C, Reynolds F. Placental transfer of anticonvulsants in the rabbit: effect of maternal protein binding and fetal flow. Placenta 1986; 7: 333–8
Wilkening RB, Anderson S, Martensson L, et al. Placental transfer as a function of uterine blood flow. Am J Physiol 1982; 242: 429–36
Vella LM, Knott C, Reynolds F. Transfer of fentanyl across the rabbit placenta — effect of umbilical flow and concurrent drug administration. Br J Anaesthes 1986; 58: 49–54
Reynolds F. Transfer of drugs across membranes. Top Rev Anaesth 1980; 1: 135–78
Biehl D, Shnider SM, Levinson G, et al. Placental transfer of lidocaine: effects of fetal acidosis. Anesthesiology 1978; 48: 409–12
Kennedy RL, Erenberg A, Robillard JE, et al. Effects of changes in maternal-fetal pH on the transplacental equilibrium of bupivacaine. Anesthesiology 1979; 51: 50–4
Datta S, Brown WU, Ostheimer GW. Epidural anesthesia for cesarean section in diabetic parturients: maternal and neonatal acid-base status and bupivacaine concentration. Anesth Analg 1981; 60: 574–8
O’Brien WF, Cefalo RC, Grissom MP. The influence of asphyxia on fetal lidocaine toxicity. Am J Obstet Gynecol 1982; 142: 205–8
Krauer B, Dayer P, Anner R. Changes in serum albumin and α1-acid glycoprotein concentrations during pregnancy: an analysis of feto-maternal pairs. Br J Obstet Gynaecol 1984; 91: 875–81
Krauer B, Nau H, Dayer P, et al. Serum protein binding of diazepam and propranolol in the feto-maternal unit from early to late pregnancy. Br J Obstet Gynaecol 1986; 93: 322–8
Hamar C, Levy G. Serum protein binding of drugs and bilirubin in newborn infants and their mothers. Clin Pharmacol Ther 1980; 28: 58–63
Petersen MC, Moore RG, Nation RL, et al. Relationship between the transplacental gradients of bupivacaine and α1-acid glycoprotein. Br J Clin Pharmacol 1981; 12: 859–62
Erkkola R, Lamintausta R, Liulkko P, et al. Transfer of propranolol and sotalol across the human placenta: their effect on maternal and fetal plasma renin activity. Acta Obstet Gynecol Scand 1982; 61: 31–4
Sioufi A, Hillion D, Lumbroso P, et al. Oxprenolol placental transfer, plasma concentrations in newborns and passage into breast milk. Br J Clin Pharmacol 1984; 18: 453–6
Meuldermans W, Woestenborghs R, Noorduin H. Protein binding of the analgesics alfentanil and sufentanil in maternal and neonatal plasma. Eur J Clin Pharmacol 1986; 30: 217–9
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bourget, P., Roulot, C. & Fernandez, H. Models for Placental Transfer Studies of Drugs. Clin. Pharmacokinet. 28, 161–180 (1995). https://doi.org/10.2165/00003088-199528020-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003088-199528020-00006