Summary
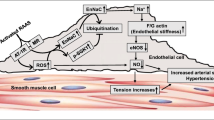
The effect of hypertension on the arterial vascular wall is characterised primarily by morphological changes to the endothelium and hypertrophy of smooth muscle cells within the arterial media. Endothelial dysfunction is manifest through increased permeability to high molecular weight compounds as well as mitogenic and vasoactive substances. At the same time, denudation of the vascular endothelium promotes platelet aggregation and subsequent release of platelet-derived growth factor (PDGF). In conjunction with endothelium- and monocyte-derived growth factors, this mitogen stimulates subintimal smooth muscle cell proliferation and migration and arterial wall thickening, resulting in a haemodynamically important increase in vascular resistance, particularly at the precapillary level. In addition, focal endothelial dysfunction allows entry of lipids into the vascular wall, thereby promoting formation of a lipid-rich fatty streak, the primary ‘early’ atherosclerotic lesion.
Most of these changes, including endothelial injury, subintimal lipid-binding, cellular proliferation and migration, platelet aggregation and PDGF release are common to both hypertensive and early atherosclerotic processes and involve the participation of calcium ions as ‘second messengers’. Thus, antihypertensive treatment with calcium antagonists may not only lead to a protective decrease in wall shear stress through a reduction in blood pressure, but may also inhibit those cellular processes within the vascular wall that are responsible for initiating atherosclerosis. Indeed, experimental as well as human studies have demonstrated a beneficial suppressant effect of calcium antagonists on the early stages of atherosclerosis.
Similar content being viewed by others
References
Horan MJ. Antihypertensive therapy and atherosclerosis. Am J Med Sci 1991; 301: 401–5.
Berk BC, Corson M. Autocrine and paracrine growth mechanisms in vascular smooth muscle. Curr Opin Cardiol 1992; 7: 739–44.
Dzau VJ, Gibbons GH, Cooke JP, et al. Vascular biology and medicine in the 1990s. Scope, concepts, potentials, and perspectives. Circulation 1993; 87: 705–19.
Rubanyi GM, Freay AD, Kauser K, et al. Mechanoreception by the endothelium: mediators and mechanisms of pressure and flow-induced vascular responses. Blood Vessels 1990; 27: 246–57.
Nabel EG. Biology of the impaired endothelium Am J Cardiol 1991; 68: 6C–8C
Cooke JP, Stamler J, Andon N, et al. Flow stimulates endothelial cells to release a nitrovasodilator that is potentiated by reduced thiol. Am J Physiol 1990; 259: H804–H12.
Loskutoff DJ, Curriden SA. The fibrinolytic system of the vessel wall and its role in the control of thrombosis. Ann N Y Acad Sci 1990; 598: 238–47.
Dzau VJ, Gibbons GH. Endothelium and growth factors in vascular remodelling of hypertension. Hypertension 1991; 18: 15–21.
Dzau VJ, Gibbons GH. Cell biology of vascular hypertrophy in systemic hypertension Am J Cardiol 1988; 62: 30G–5G
Davies PF, Tripathi SC. Mechanical stress mechanisms and the cell. An endothelial paradigm. Circ Res 1993; 72: 239–45.
Holtz J. The cardiac renin-angiotensin system: physiological relevance and pharmacological modulation. Clin Investig 1993; 71: 25–34.
Kreutz R, Ganten D. Cell biology in hypertension. Curr Opin Cardiol 1991; 6: 680–5.
Henry PD. Atherogenesis, calcium and calcium antagonists. Am J Cardiol 1990; 66: 31–61.
Venkata C, Ram S. Antiatherosclerotic and vasculoprotective actions of calcium antagonists. Am J Cardiol 1990; 66: 291–321.
Yang Z, Noll G, Lüscher TF. Calcium antagonists differently inhibit proliferation of human coronary smooth muscle cells in response to pulsatile stretch and platelet-derived growth factor. Circulation 1993; 88: 832–6.
Etingin OR, Haijar DP. Calcium channel blockers enhance cholesteryl ester hydrolysis and decrease total cholesterol accumulation in human aortic tissue. Circ Res 1990; 66: 185–90.
Rafflenbeul W, Riedel M. Update on cardiac catheterization and coronary arteriography. Curr Opin Cardiol 1993; 8: 572–80.
Loaldi A, Polese A, Montorsi P, et al. Comparison of nifedipine, propranolol and isosorbide dinitrate on angiographic progression and regression of coronary arterial narrowings in angina pectoris. Am J Cardiol 1989; 64: 433–9.
Gottlieb SO, Brinker JA, Mellits ED, et al. Effect of nifedipine on the development of coronary bypass graft stenoses in high-risk patients: a randomized double-blind placebo-controlled trial [abstract]. Circulation 1989; 80 Suppl. II: II228.
Lichtlen PR, Hugenholtz PG, Rafflenbeul W, et al, on behalf of the INTACT group of investigators. Retardation of angiographie progression of coronary artery disease by nifedipine. Lancet 1990; 335: 1109–13.
Waters D, Lespérance J, Francetich M, et al. A controlled clinical trial to assess the effect of a calcium channel blocker on the progression of coronary atherosclerosis. Circulation 1990; 82: 1940–53.
Kaplan NM. Arterial protection: a neglected but crucial therapeutic goal Am J Cardiol 1990; 66: 36C–8C.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Rafflenbeul, W. Hypertension Treatment and Prevention of New Atherosclerotic Plaque Formation. Drugs 48 (Suppl 1), 11–15 (1994). https://doi.org/10.2165/00003495-199400481-00005
Published:
Issue Date:
DOI: https://doi.org/10.2165/00003495-199400481-00005